Claim Landing Page
Streamlined access to all claims with a clear to-do panel for priority task visibility.

Click to View Image


For Phase I of the Claim Processing Application, I led the design of a 0→1 MVP that reimagined how NARS adjusters handled claims across the legacy Claims Cube (C3) environment.
The existing C3 experience required adjusters to move through disconnected workflows, scattered claim details, manual documentation patterns, and inconsistent task handling. The MVP replaced that structure with a unified claims workspace that centralized claim handling, documents, communication, to-dos, and parties into a clearer, more scalable operational model.
The goal was not simply to modernize the interface. It was to reduce context switching, improve workflow predictability, support compliance-heavy claim operations, and create a foundation the product team could confidently expand beyond MVP.
As the UX/UI designer, I led the end-to-end design of the MVP — from discovery, workflow mapping, and research synthesis through Figma interface design, prototyping, design systems, and engineering handoff.
I partnered with product, engineering, business analysts, QA, stakeholders, and a junior designer to turn complex claim workflows into structured, accessible, Angular-ready product patterns that supported MVP delivery and future platform growth.
67%
Usability Increase
Centralized workflows and clearer hierarchy reduced friction across daily claim work.
71%
Satisfaction Uplift
Predictable patterns and stronger task visibility improved adjuster confidence.
80%
Development Velocity
Reusable components and Angular-ready patterns accelerated MVP delivery.
45%
Support Reduction
Guided workflows and clearer documentation reduced common support needs.
“The progress on the Claim Processing Application has been transformative for our adjusters. Workflows feel clearer, faster, and far more predictable than anything we’ve had before. For the first time, teams can move through claims without the constant friction of switching between tools or second-guessing next steps. We’re extremely pleased with where the product is today — and even more excited about the strong, scalable foundation it gives us for continued growth.”
Michael Reynolds – Senior Operations Stakeholder
I led the UX strategy and UI design for a 0→1 enterprise claims platform MVP that replaced disconnected Claims Cube workflows with a centralized, WCAG 2.1 AA–aligned adjuster workspace. The product unified claim handling, documentation, communication, and task management while introducing a scalable Figma design system aligned to Angular implementation.
The MVP delivered a 67% increase in usability, 71% uplift in user satisfaction, 80% faster development velocity, and a 45% reduction in support tickets by improving workflow clarity, reducing context switching, and creating reusable product patterns for future growth.
Claims processing depended heavily on disconnected workflows within the legacy Claims Cube (C3) experience. Adjusters moved between siloed screens, manual workarounds, spreadsheets, and inconsistent claim handling patterns that slowed daily work, reduced visibility, and increased operational risk across the claim lifecycle.
The challenge was not just interface modernization. The product needed to translate complex, compliance-driven claim work into a structured experience that reduced ambiguity, improved task predictability, and helped adjusters manage high-volume workloads with greater confidence.
No scalable product structure, workflow model, or reusable UI system existed to support the new MVP.
Claims, documents, communication, and tasks lived across separate C3 patterns, forcing users to rebuild context.
Duplicate entry, repetitive steps, and inconsistent claim records created avoidable effort and risk.
Inconsistent workflow patterns made it harder for adjusters to know what needed attention next.
Claim status, ownership, handoffs, and supporting documentation were difficult to track across teams.
Without clear structure and trust, users were less likely to adopt a new platform with confidence.
This C3 claim screen shows the kind of dense, disconnected experience adjusters worked through daily. Key claim details, documents, activities, policy data, and next steps were visible in pieces, but the interface did not clearly guide users toward what needed attention first.
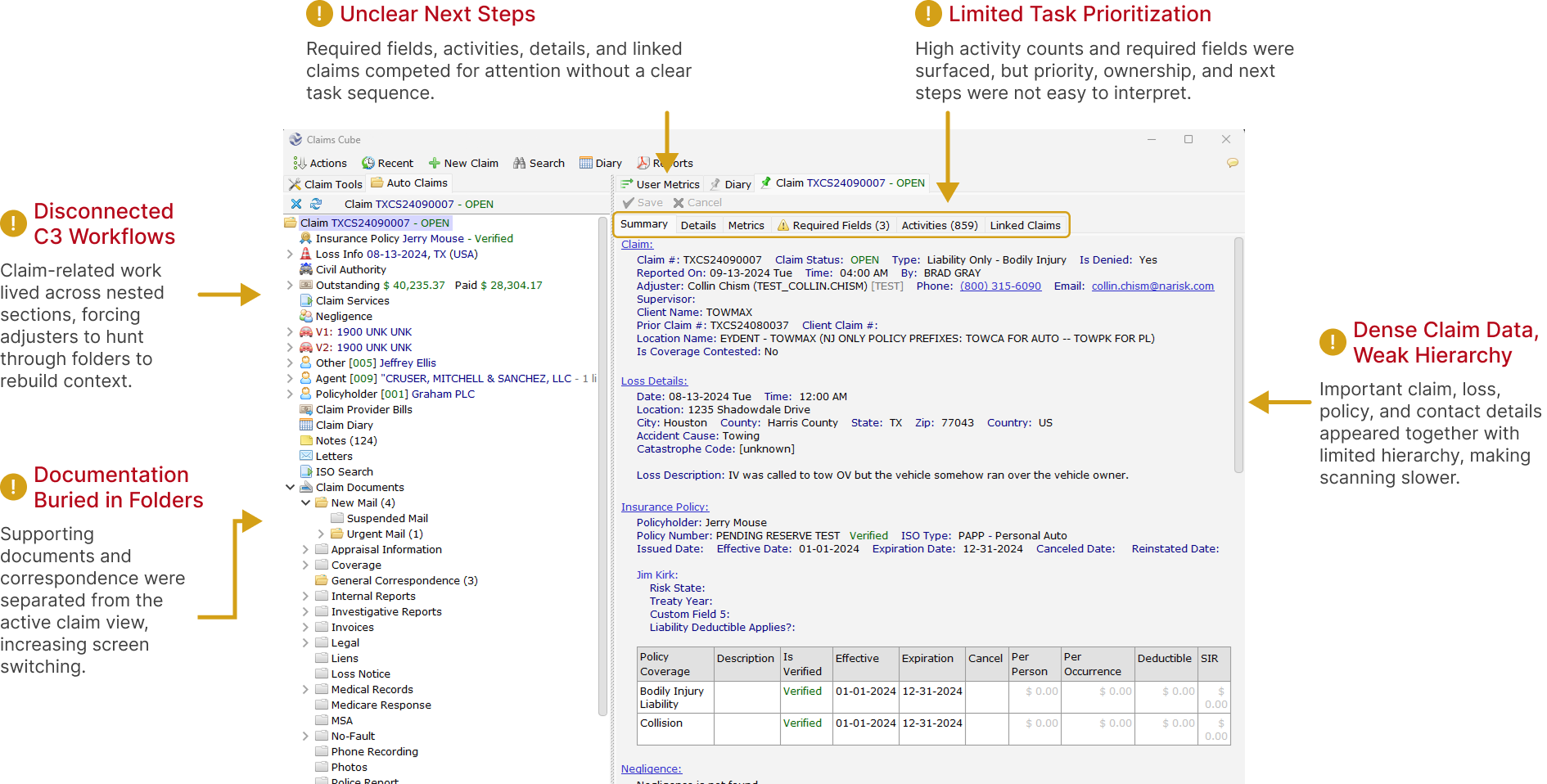
Annotated C3 screen showing how claim context, documentation, activities, and required tasks were technically available, but difficult to scan, prioritize, and act on efficiently.
The goal for Phase I was to move beyond the limitations of C3 and define a clearer, more reliable way for adjusters to manage daily claim work.
Instead of treating the MVP as a surface-level redesign, we focused on the behaviors that created the most friction: finding claim context, understanding what needed attention, documenting work, and coordinating across roles.
These goals helped the team prioritize clarity, consistency, and workflow confidence before moving into detailed interaction design.
Create a consistent foundation users could trust and the product team could expand over time.
Reduce screen switching by giving adjusters a single place to stay oriented around active claim work.
Minimize repetitive work through smart defaults, validation patterns, and clearer system feedback.
Support in-context notes, structured call logs, message history, and audit-ready claim documentation.
Guide junior adjusters clearly while helping experienced adjusters move quickly through claim volume.
Make claim status, ownership, handoffs, and next steps easier to see across teams and roles.
Once the goals were aligned, we organized the MVP around six core areas of the claim experience. This created a shared product model for what Phase I needed to support before detailed interaction design began.
A shared model for structuring the MVP around daily adjuster work.
Claims
Claim status, intake, lifecycle context
To-Dos
Task sequence, required actions, follow-ups
Claim Details
Loss details, policy data, claim context
Documents
File access, records, supporting documentation
Communication
Calls, notes, messages, claim history
Parties
People, roles, ownership, contacts
With the MVP scope defined, the next step was turning the goals into a clear design strategy that could guide product decisions, interaction patterns, and engineering alignment.
We focused the approach around four strategic moves: unify daily claim work, reduce cognitive load, build trust through clearer workflows, and scale the system through reusable patterns.
Design Moves
Connected core claim work into one model so adjusters could maintain context across tasks, documents, and communication.
Design Moves
Simplified dense claim information so users could scan, prioritize, and act with less effort.
Design Moves
Made required actions, records, and handoffs clearer so adjusters could work with more confidence and fewer missed steps.
Design Moves
Created reusable patterns that supported MVP consistency while giving the product team a foundation for growth.
Rather than translating C3 directly into a new interface, we reframed the experience around how adjusters needed to move through active claim work.
Legacy C3
Users rebuilt context across separate screens and patterns.
NARS Core MVP
Core claim work moved into one structured workflow model.
Because this was a 0→1 product effort, discovery focused on understanding how adjusters actually moved through claim work inside the existing C3 environment.
We used Maze surveys, interviews, workflow observation, and persona development to uncover where work slowed down, where context broke apart, and where users relied on manual tracking to complete critical claim tasks.
Research revealed recurring issues around context switching, duplicate data entry, limited task visibility, unclear ownership, and inconsistent documentation patterns. These findings shaped the MVP’s navigation model, workflow structure, and prioritization strategy.
We used a brief Maze survey to establish a baseline view of how junior and senior adjusters moved through claim work.
The goal was to identify where time was lost, where workflows felt fragile, and which patterns created the most friction across high-volume, compliance-driven tasks.
The responses confirmed that the existing C3 experience was slowing users down through repeated context switching, duplicate entry, unclear next steps, and difficulty locating supporting documentation during active claim work.
Building on the survey findings, we conducted one-on-one interviews with adjusters and team leads to understand the behaviors behind the data.
These conversations clarified how role, experience level, claim volume, and compliance pressure shaped day-to-day workflows. They also helped guide early decisions around task visibility, document access, guided actions, and claim-level communication.
A clear pattern emerged: junior and senior adjusters needed the same foundation of clarity, but their friction showed up differently. Junior adjusters needed guidance and reassurance. Senior adjusters needed speed, visibility, and fewer interruptions.
Junior and senior adjusters shared the same need for clarity, but their day-to-day friction showed up differently.
Junior Adjusters
Senior Adjusters
To keep product decisions grounded in real adjuster needs, we distilled the research into two primary personas: junior adjusters and senior adjusters.
Together, these personas helped frame the MVP around two critical needs: confidence for newer adjusters and speed plus visibility for experienced adjusters. They became decision-making tools for navigation, task sequencing, documentation patterns, and workflow density.


After synthesizing survey results, interviews, and persona insights, we mapped the full claims workflow journey in Miro from intake through investigation, evaluation, resolution, and closure.
This exercise clarified where adjusters lost time, where context broke down, and where the experience created uncertainty instead of momentum.
The journey exposed recurring breakdowns around documentation access, communication tracking, manual prioritization, ownership visibility, and claim handoffs across the legacy C3 structure.
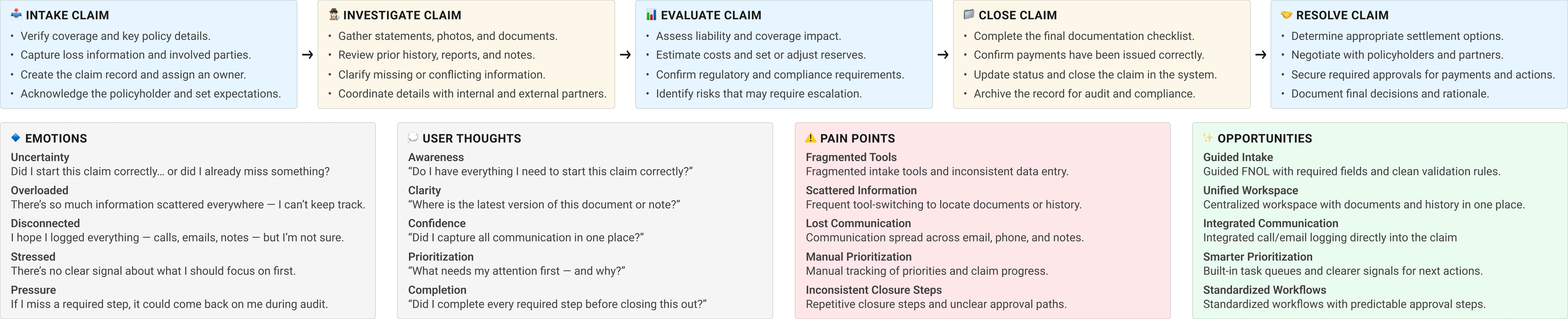

I facilitated a structured discovery workshop in FigJam with product, stakeholders, business analysts, engineering, and adjuster team leads to translate research findings into actionable MVP priorities.
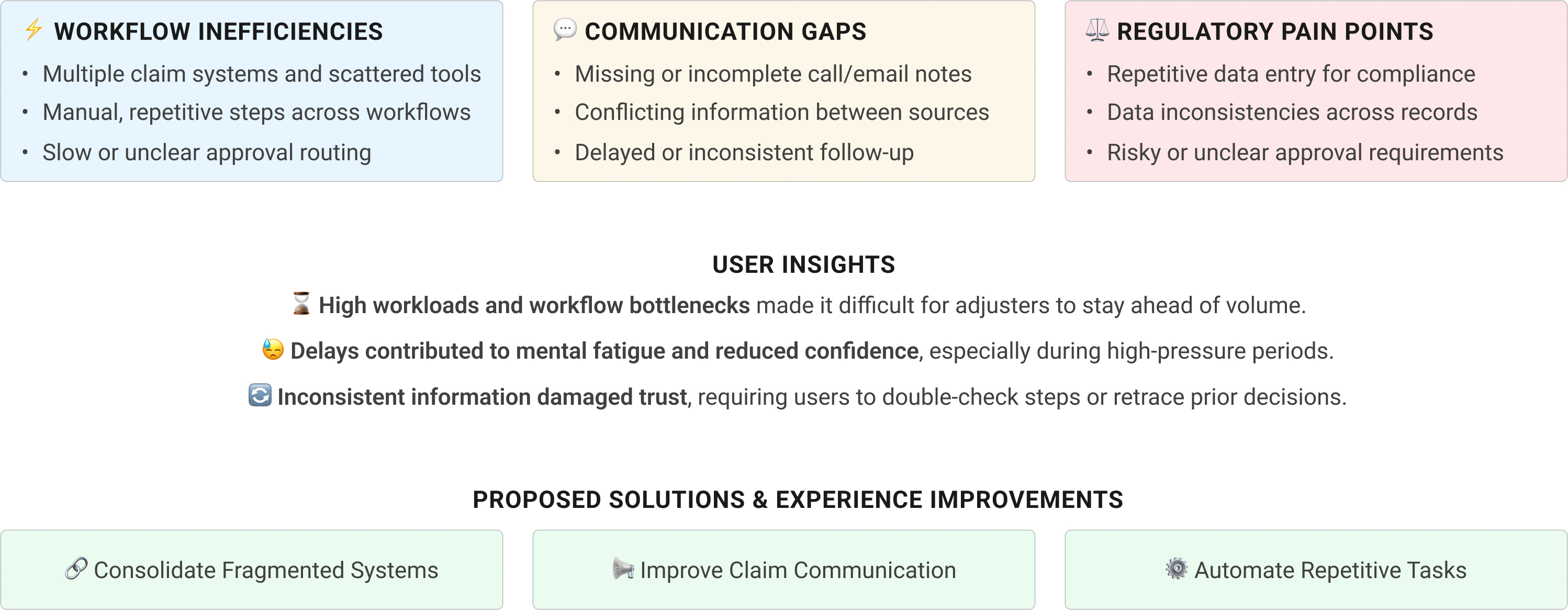
The workshop helped the team connect what we heard in research to the parts of the C3 experience that created the most friction: disconnected workflow areas, unclear next steps, documentation risk, and limited claim context.
Four priorities emerged: unify daily claim work, clarify high-value tasks, strengthen documentation trust, and create reusable system patterns for MVP delivery.
Using FigJam to organize early ideas, ideation focused on turning research and workshop priorities into a scalable product structure that supported real adjuster behavior without recreating the limitations of C3.
Early concepts explored how users would enter the platform, manage claim work, access documentation, complete tasks, and maintain context across high-volume workflows.
Early concepts leaned heavily toward operational dashboards, but stakeholder reviews exposed unnecessary complexity for the MVP.
I pushed the team toward a more focused claim-first model that prioritized scannability, task sequencing, and faster decision-making over broad dashboard visibility. This tradeoff reduced scope risk while creating a stronger foundation for the workflows adjusters used most often.
Sketching in FigJam helped translate workshop priorities into structure before the team invested in higher-fidelity screens. We explored low-fidelity directions for the claim landing page, active claim views, to-do handling, document access, and communication patterns.
Streamlined access to all claims with a clear to-do panel for priority task visibility.

Click to View Image
Paired high-level claim context with a dedicated documents view to reduce screen switching.

Click to View Image
Introduced tabbed navigation with persistent document access to keep claim context in view.
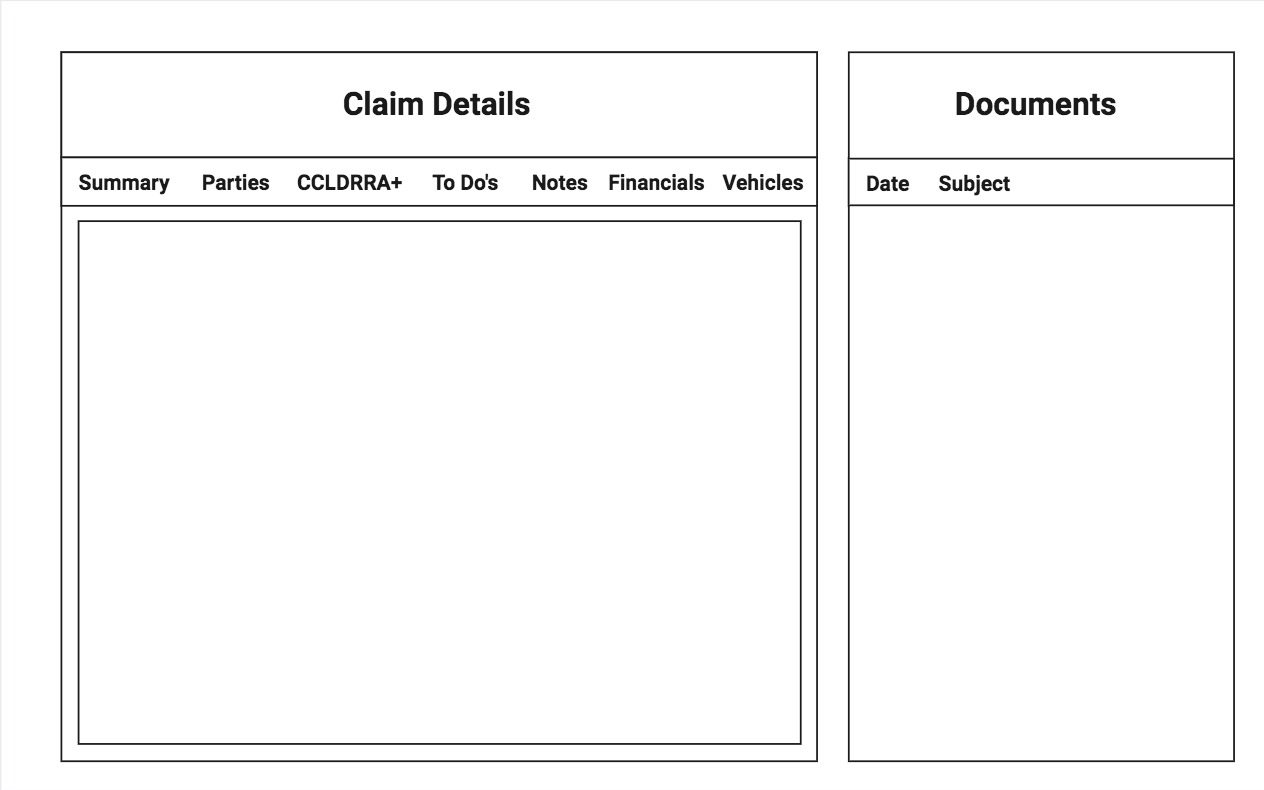
Click to View Image
Once the core workflow structure was aligned, we moved into high-fidelity wireframes in Figma to validate layout behavior, navigation clarity, and task sequencing before final UI design.
These wireframes gave stakeholders and engineering a shared view of how the product would function across realistic claim scenarios. Priority workflows included claim intake, task handling, claim details, and document management.
This phase surfaced structural improvements early, reduced downstream engineering rework, and clarified how the product should behave under high-volume claim activity.
Consolidated active claims and to-do visibility into a cleaner, more focused workspace.
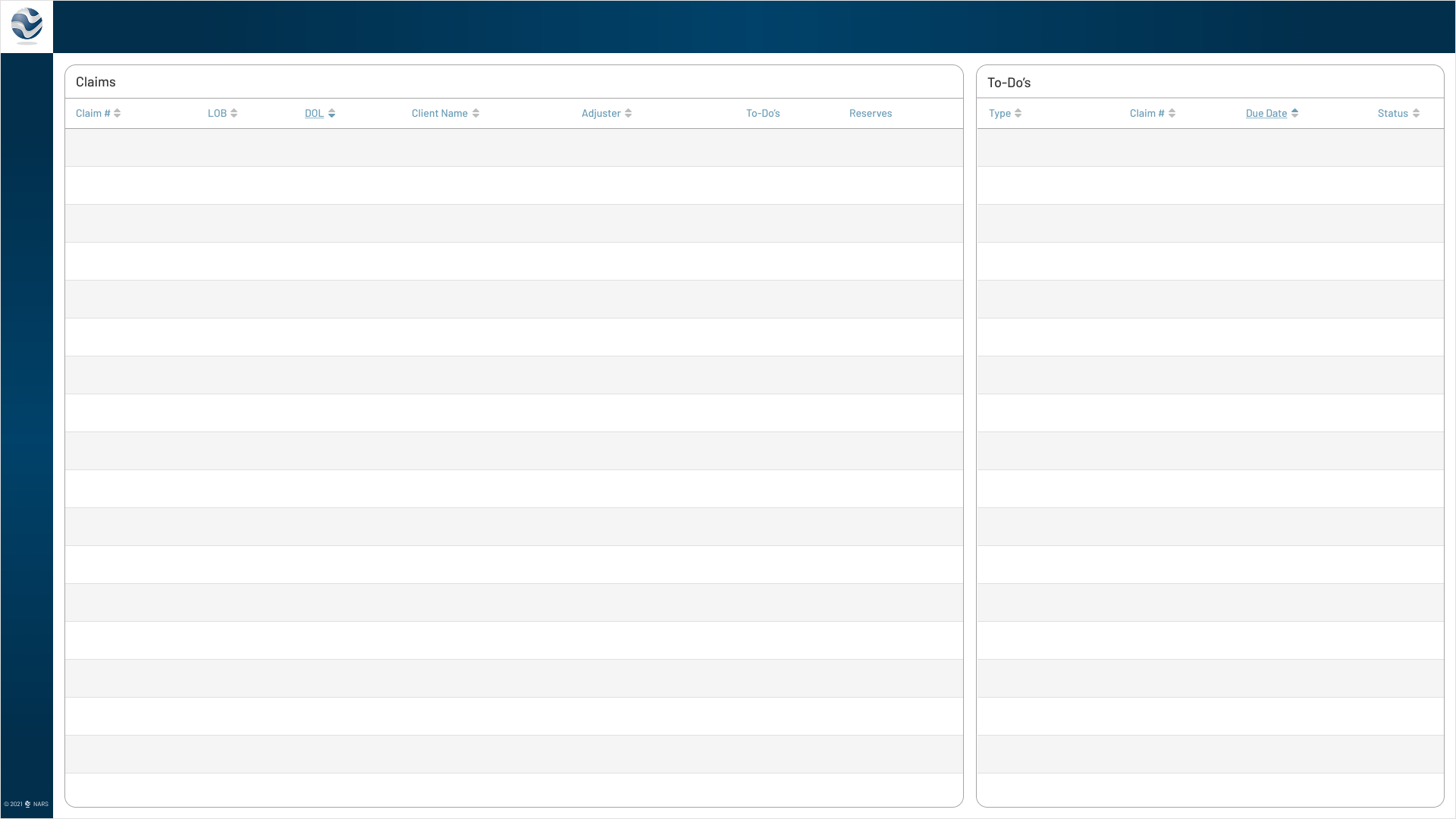
Click to View Image
Surfaced required task fields in a focused view to reduce confusion and improve completion speed.
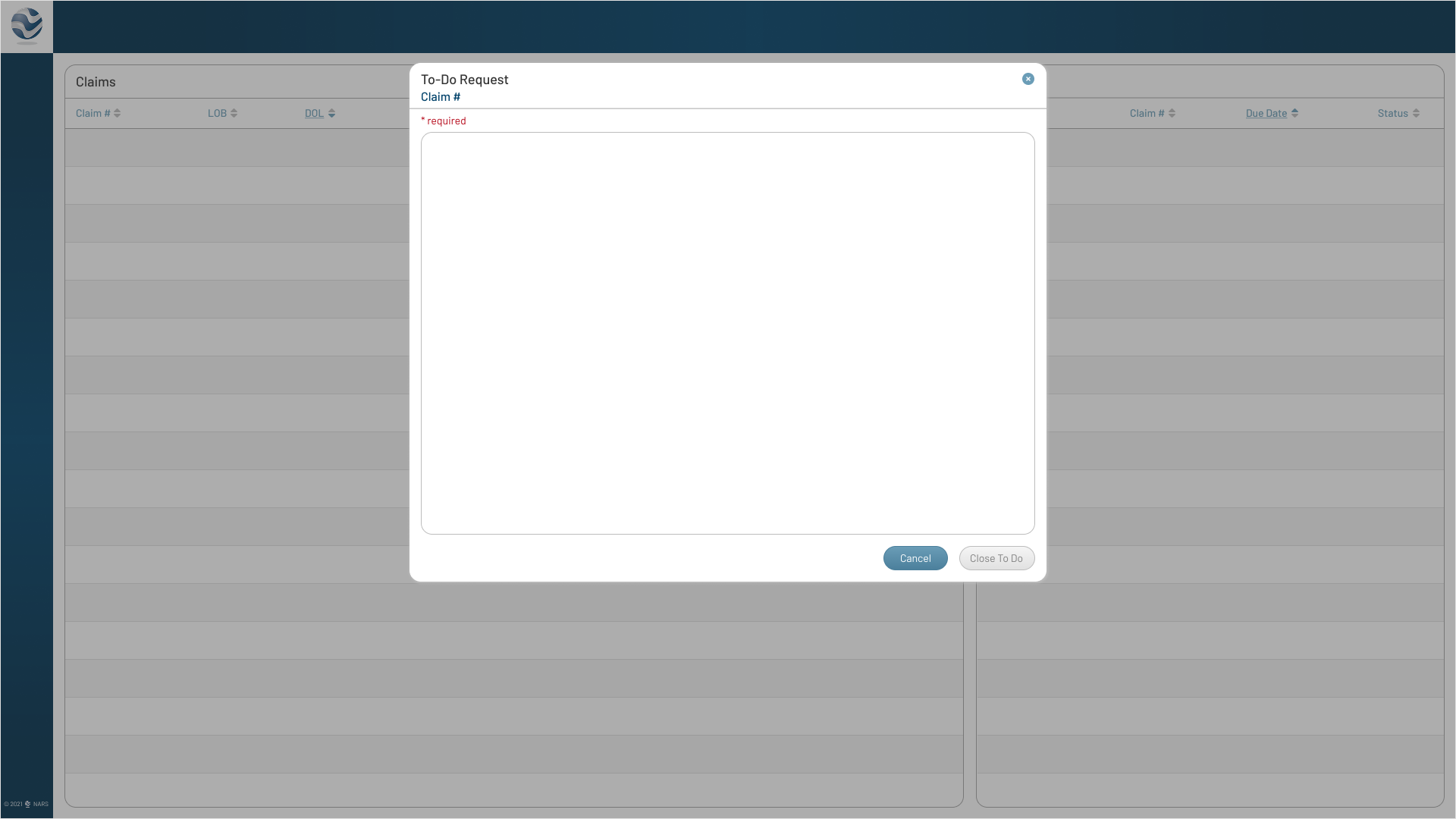
Click to View Image
Paired summary data with documentation access to support faster decisions and fewer screen jumps.
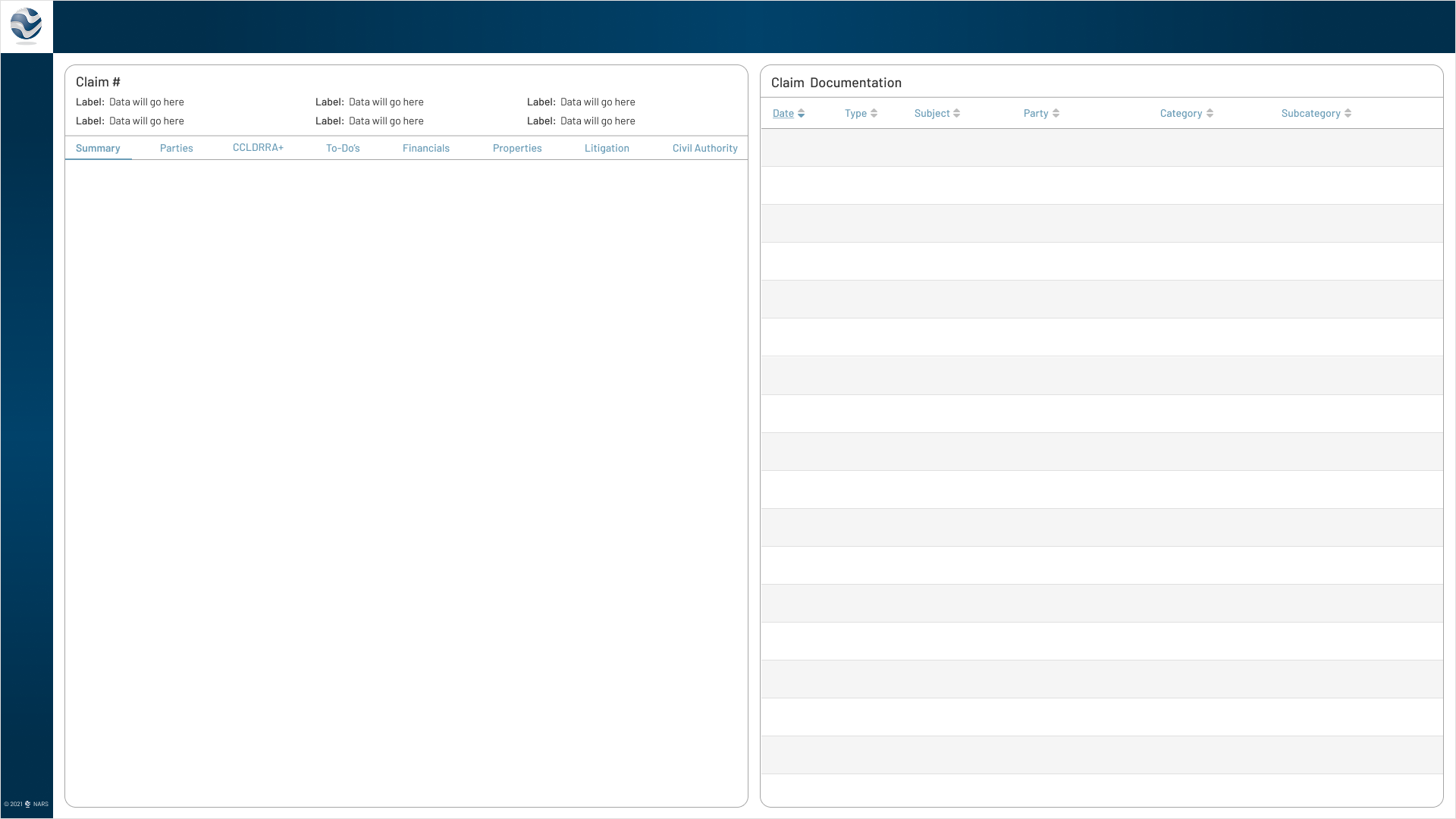
Click to View Image
Because the MVP was being built inside a regulated claims environment, validation focused on reducing workflow risk without slowing delivery.
Instead of running large-scale usability studies, we used targeted walkthroughs with Unit Managers, product leadership, and operational stakeholders to evaluate the highest-impact claim workflows before engineering implementation accelerated.
Feedback was reviewed through an MVP lens: what needed to be refined for launch, what could be handled through clearer interaction patterns, and what should move into Phase II.
We ran scenario-based walkthroughs using realistic claim workflows and Maze-supported feedback prompts to evaluate how adjusters completed tasks, reviewed documents, managed communication, and navigated claim details inside the MVP experience.
The walkthroughs focused less on visual polish and more on workflow clarity, task confidence, information accessibility, and whether users could complete core actions without unnecessary interruption.
Based on validation feedback, we made a focused set of refinements that improved day-to-day usability without changing the MVP architecture.
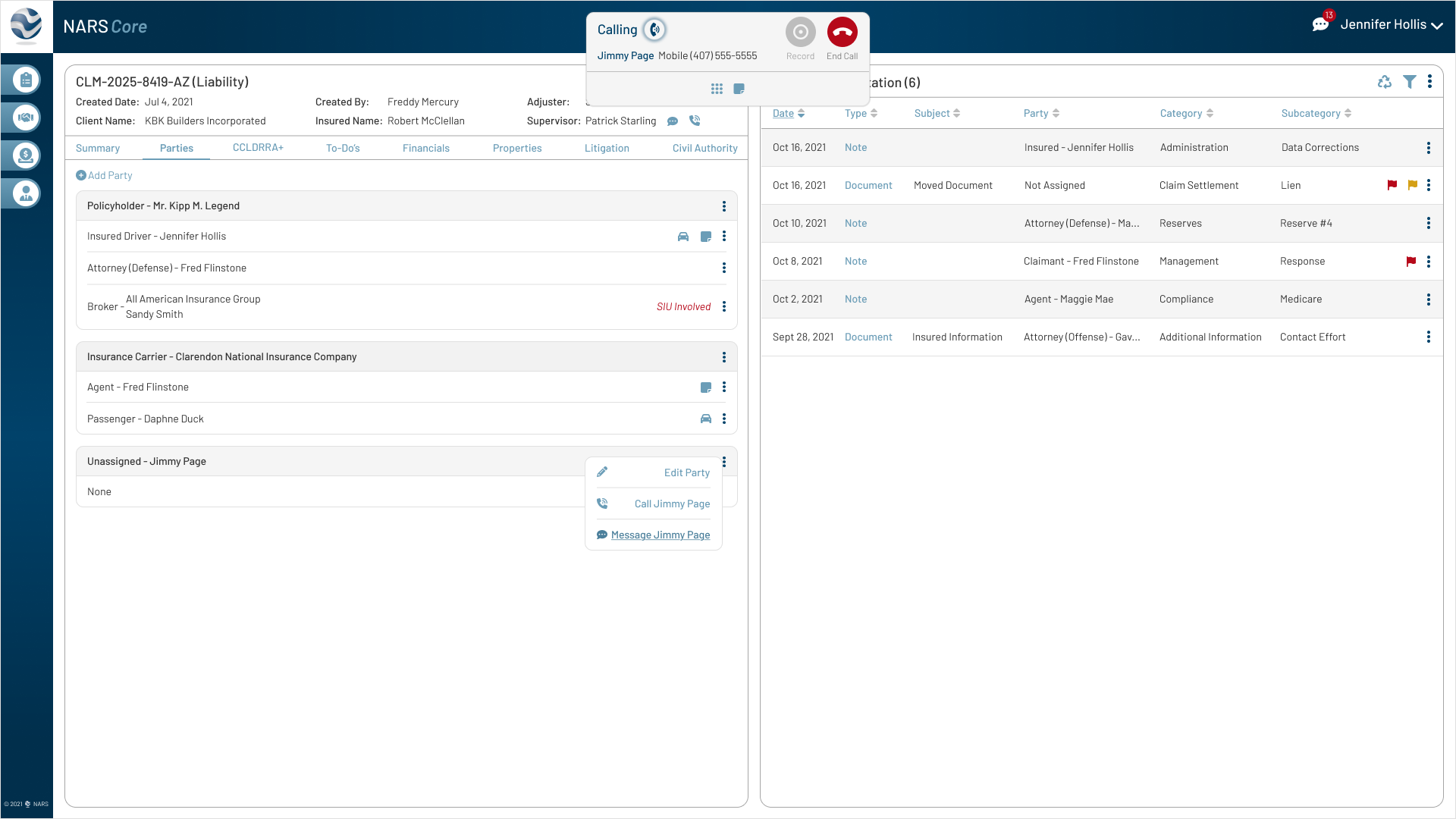
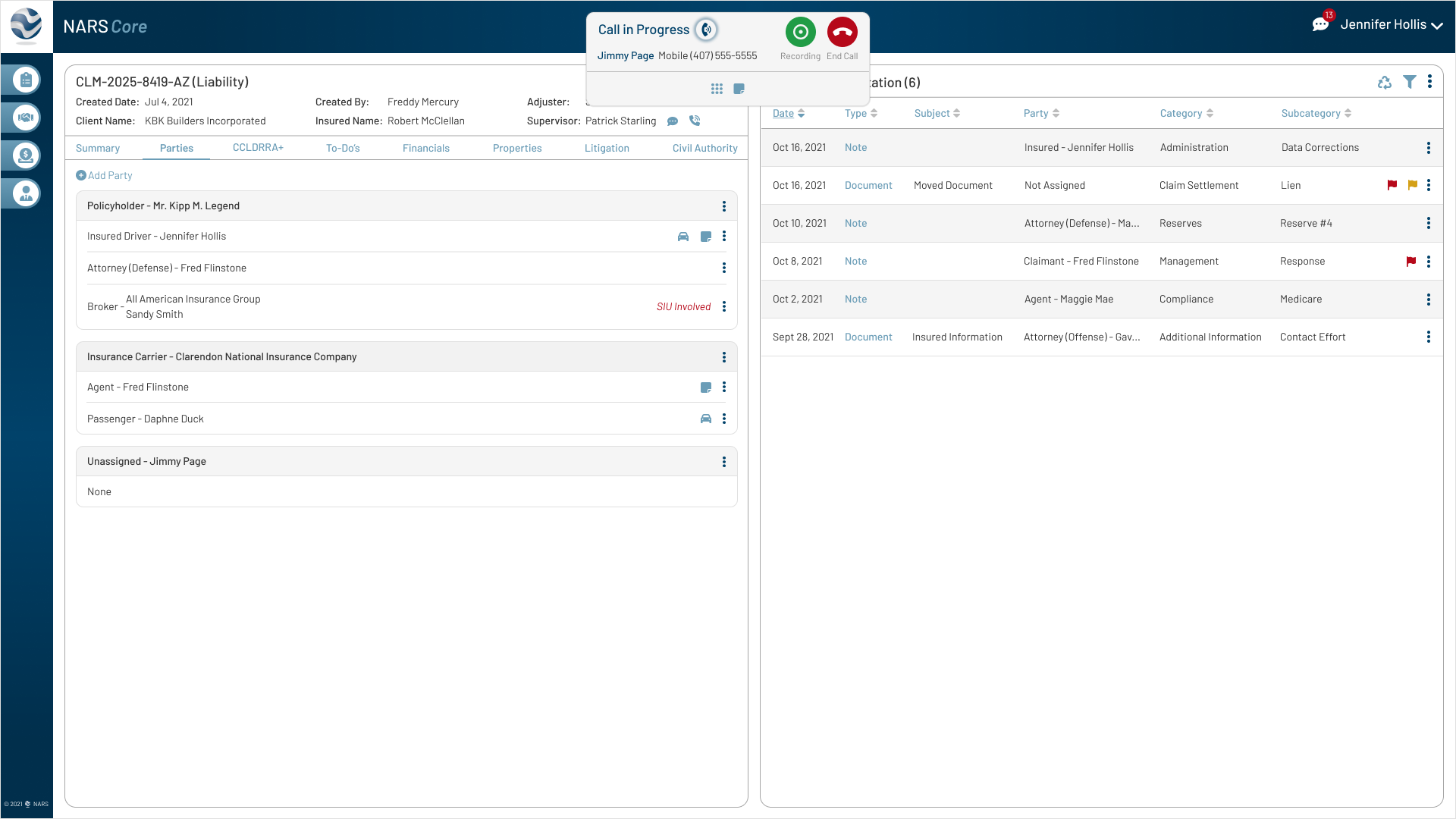
These updates addressed three workflow gaps uncovered during testing: capturing call notes in context, connecting notes to documents, and keeping multi-user communication traceable.
Feedback
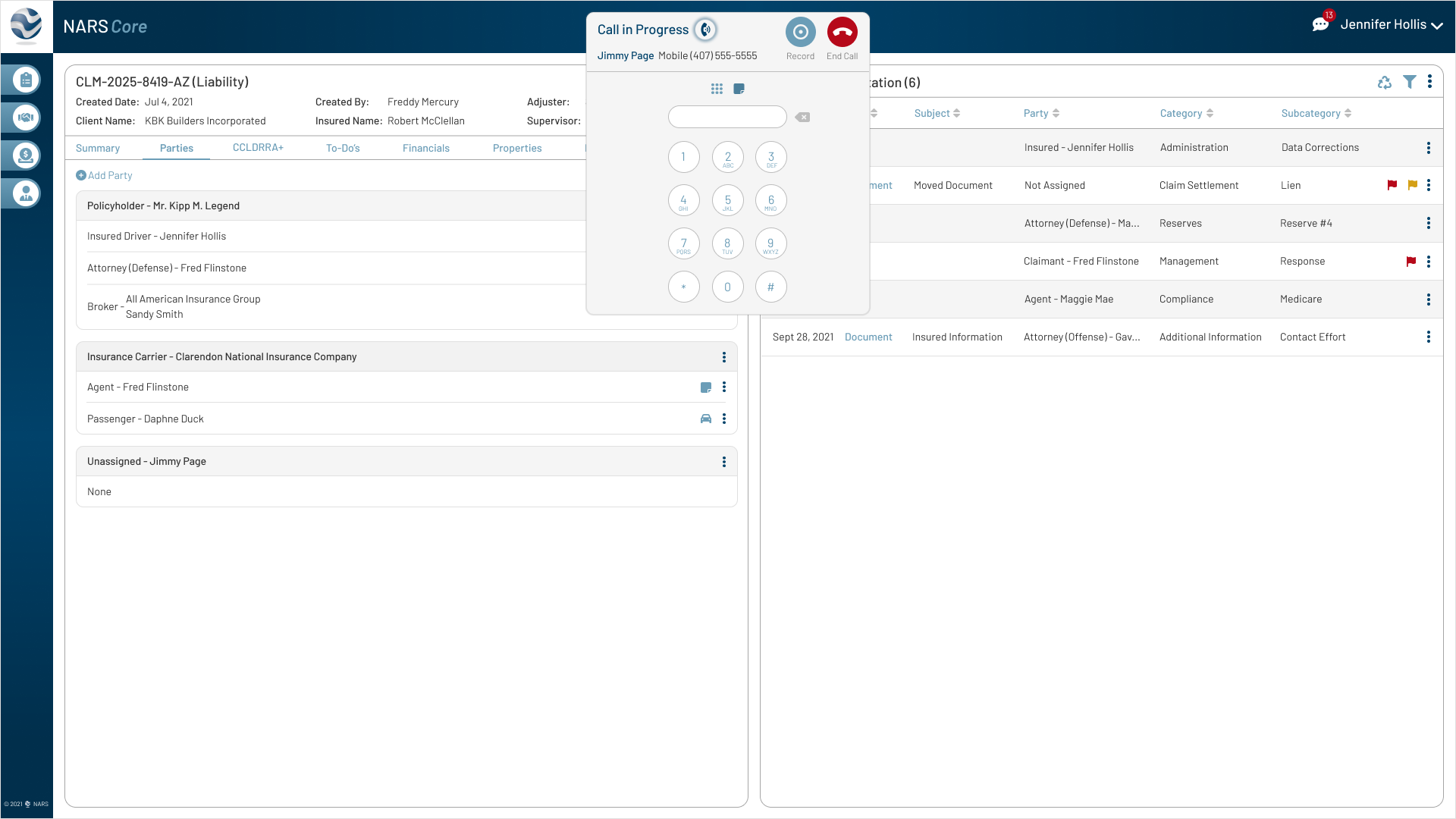
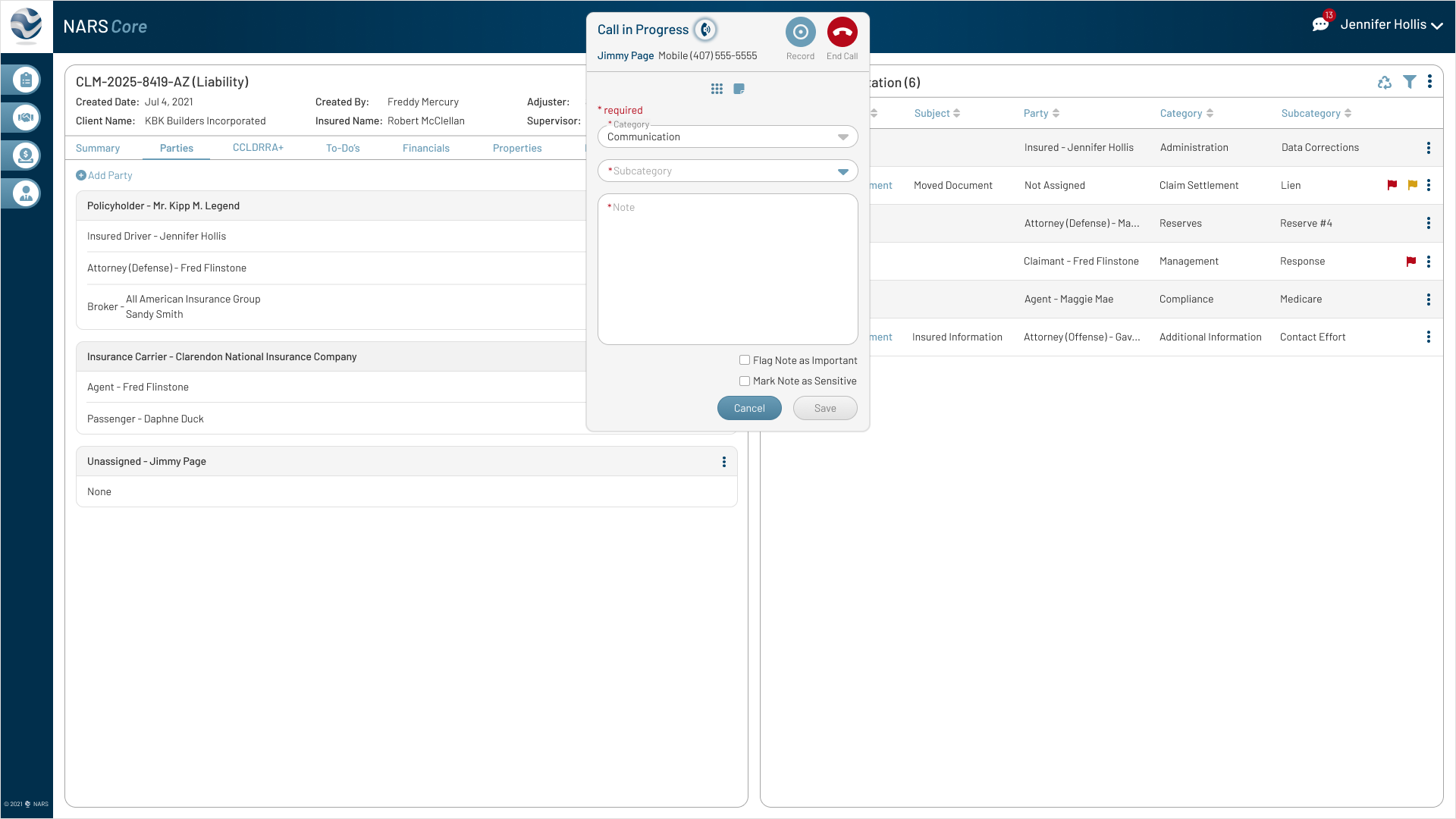
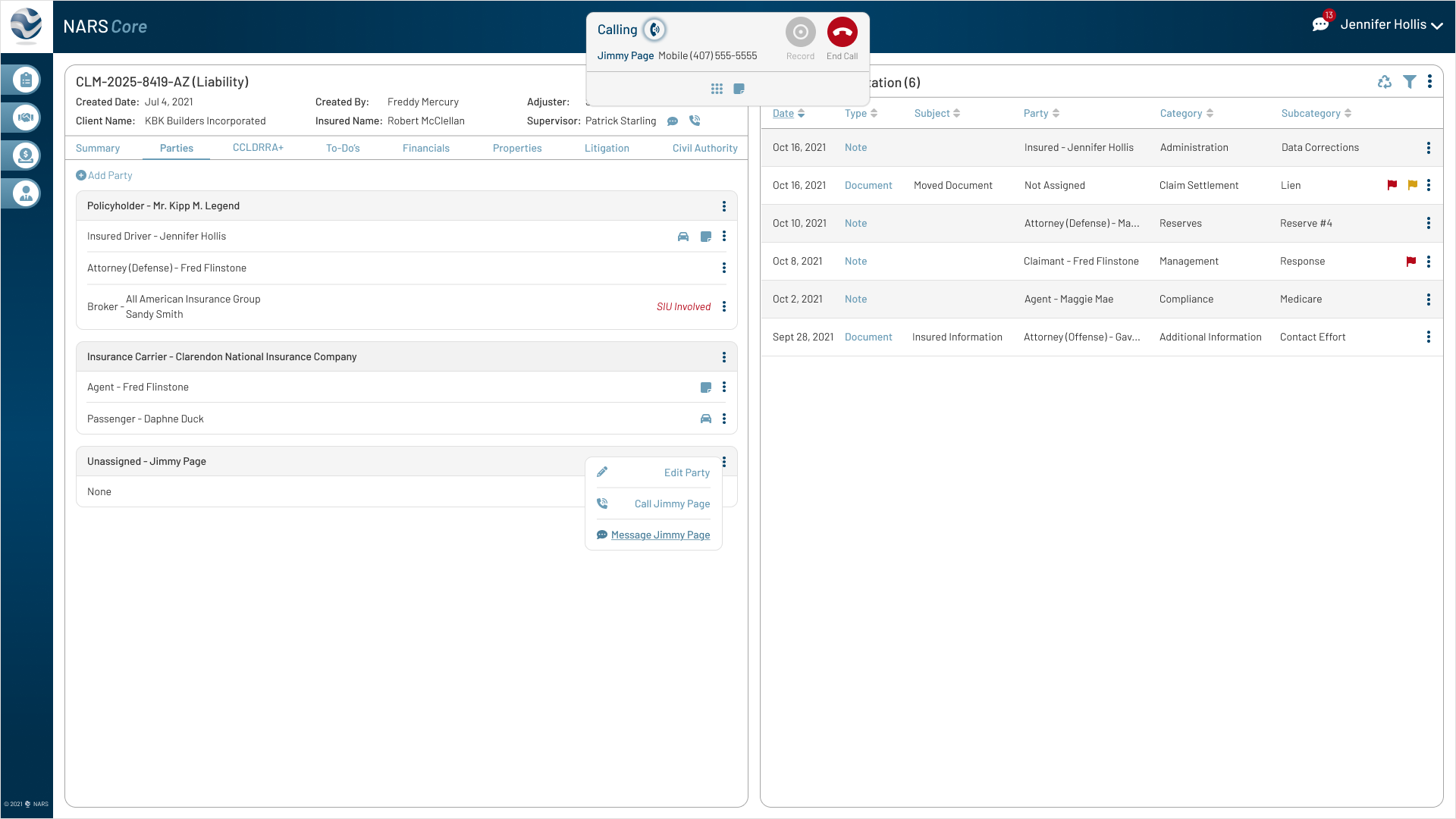
Adjusters needed to capture call notes in real time without leaving the active claim.
Iteration
Added an inline note field and dial pad to support call documentation directly inside the claim workflow.
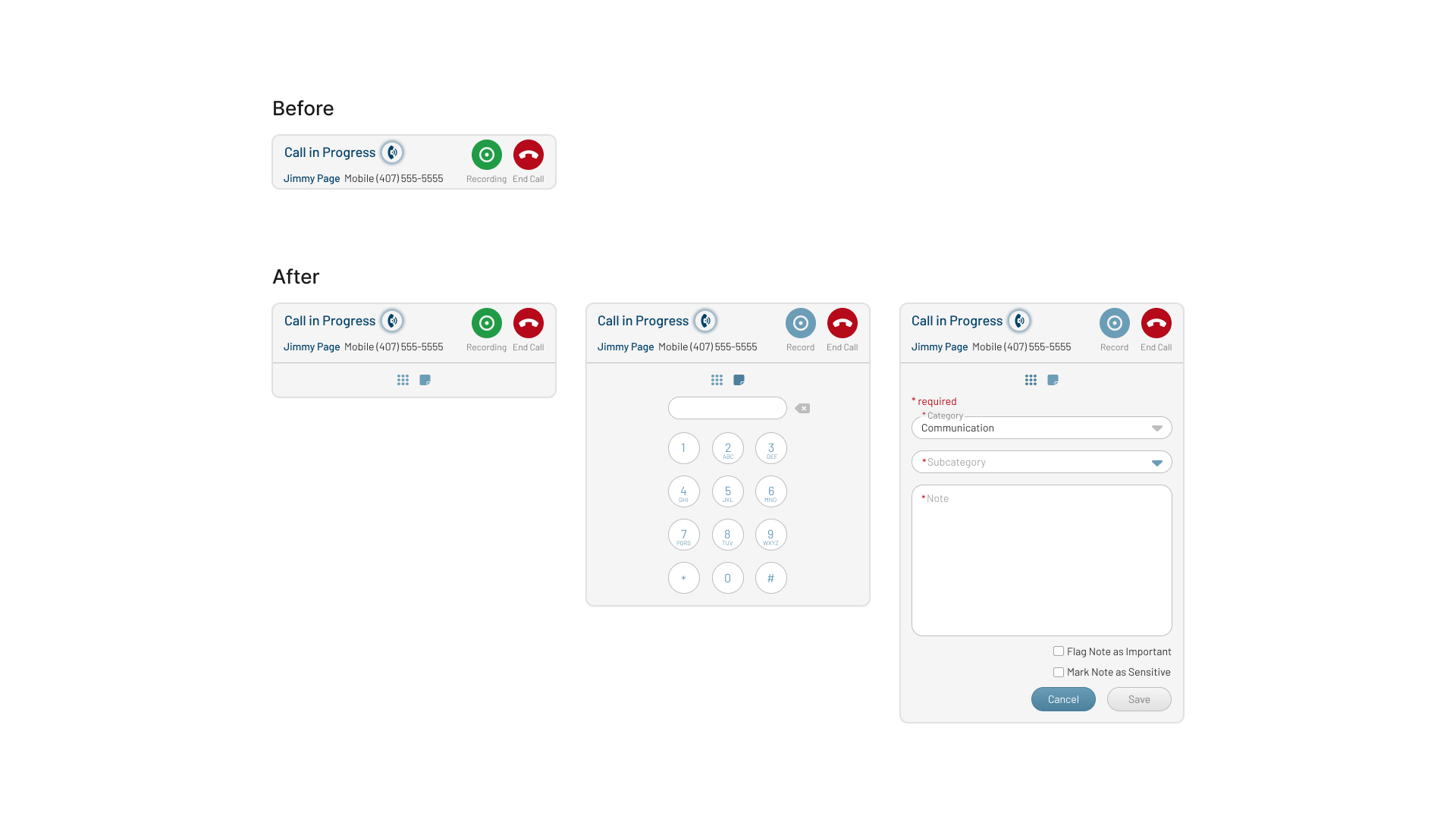
Click to View Image
Feedback
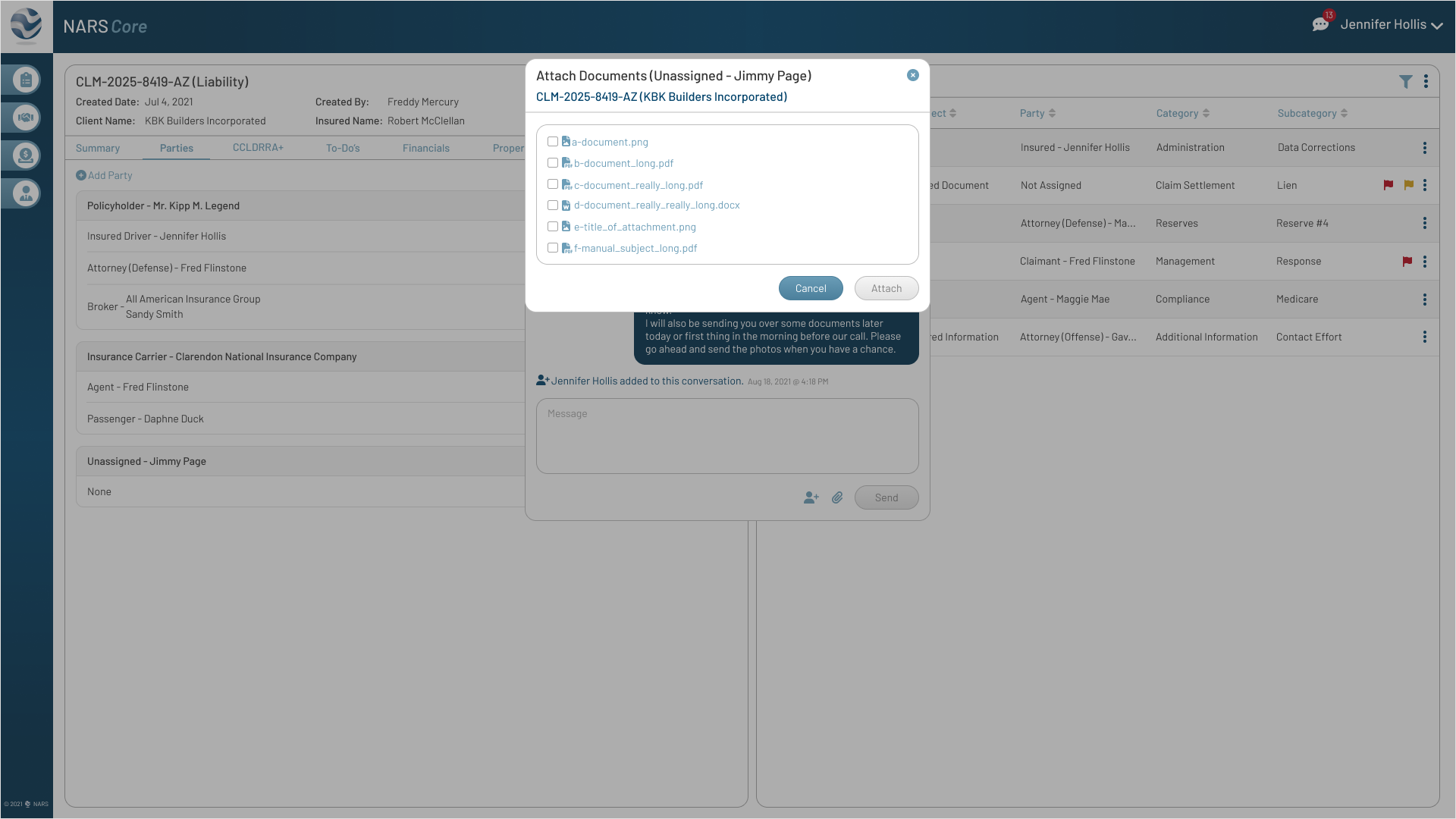
Notes stored only at the claim level made it harder to connect them to specific files.
Iteration
Added note entry directly into the Documents workflow to strengthen audit trails and keep file context easier to review.
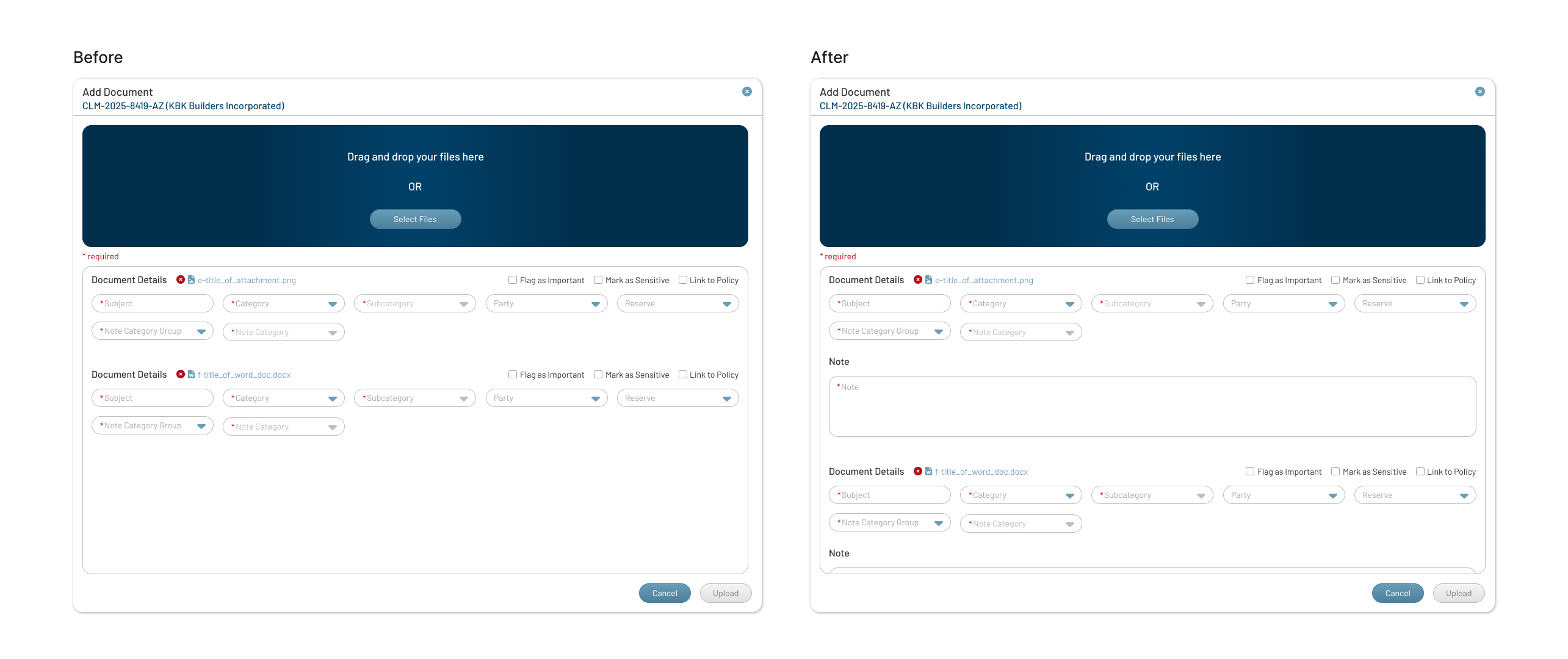
Click to View Image
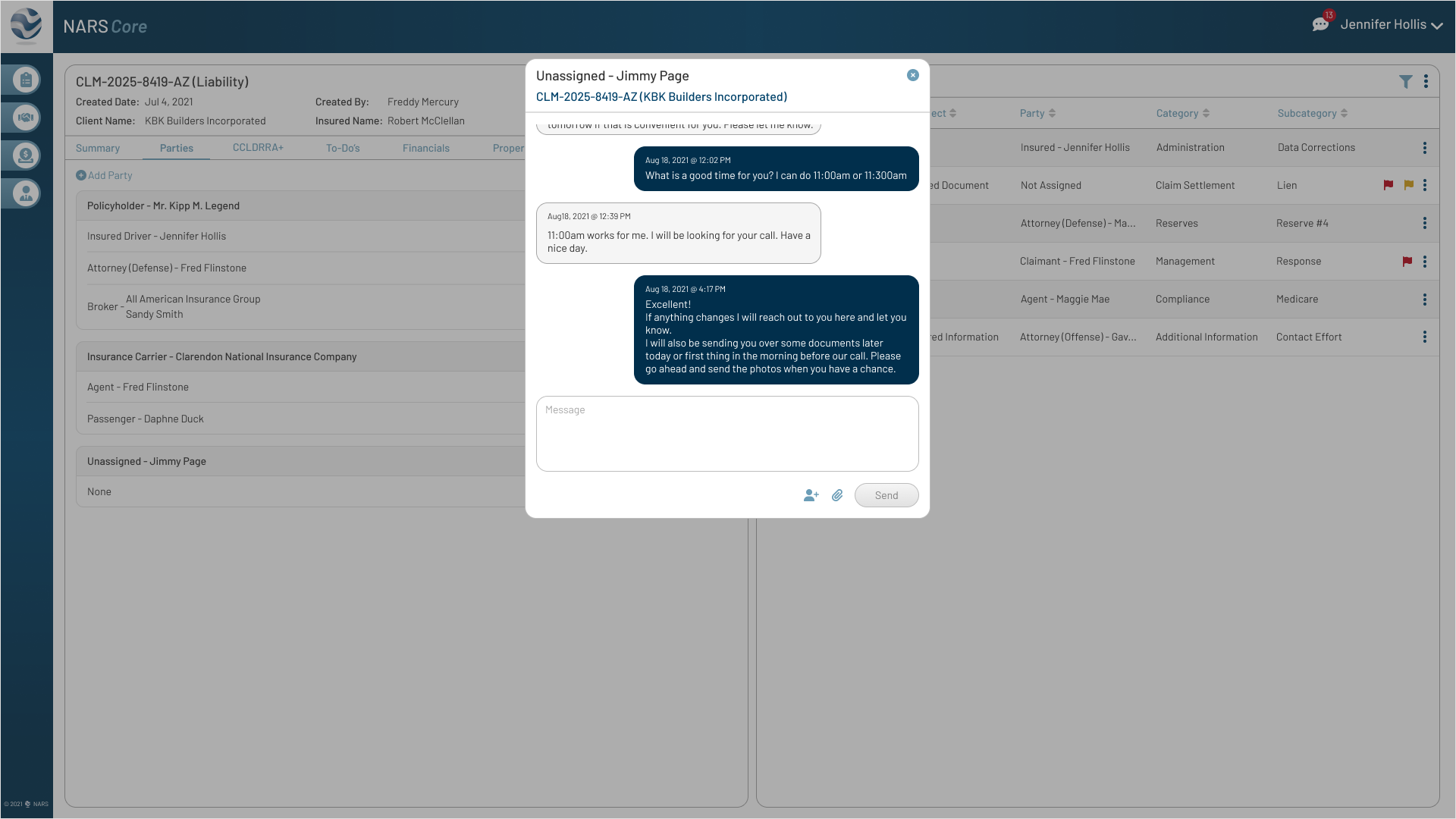
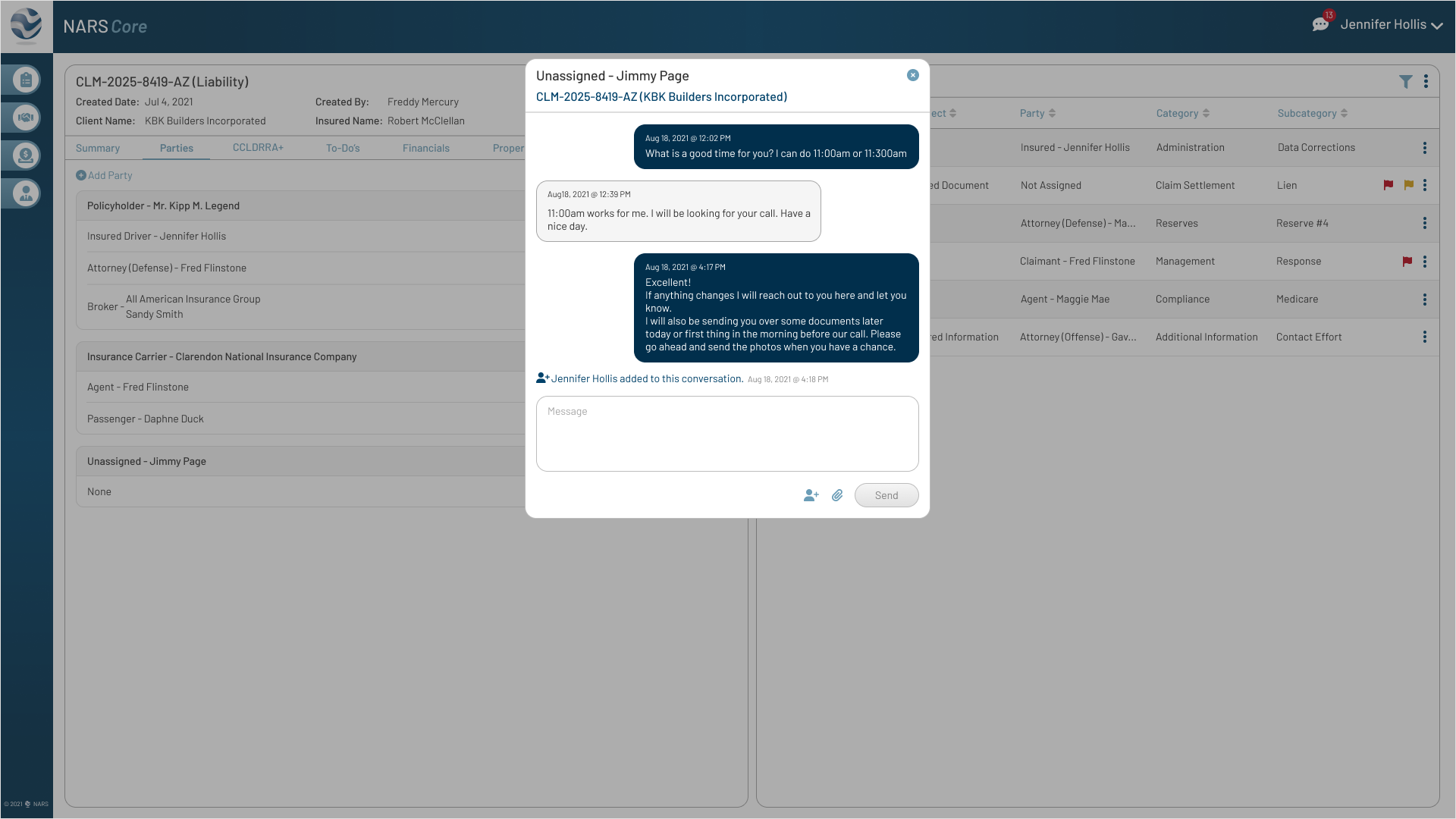
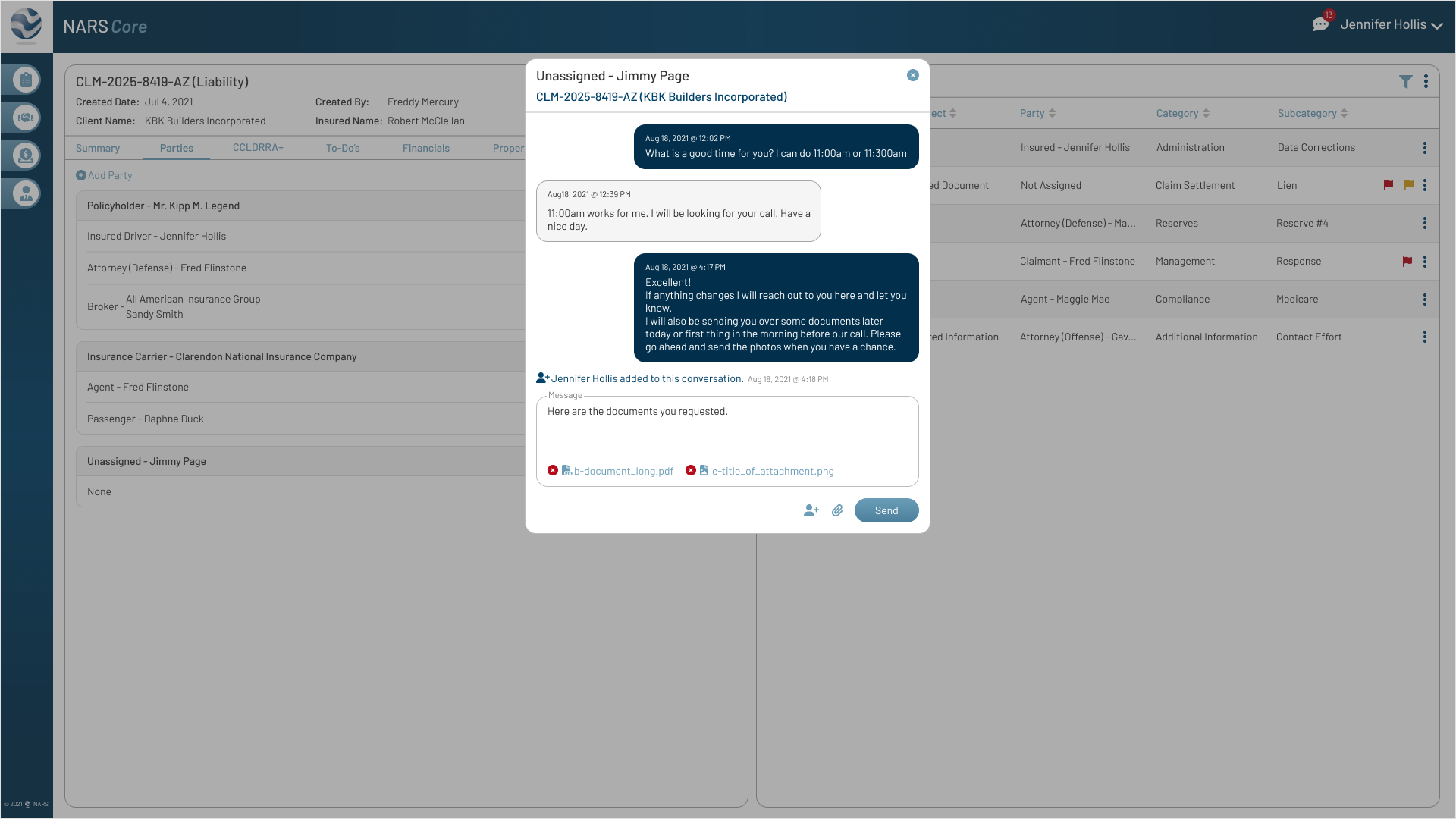
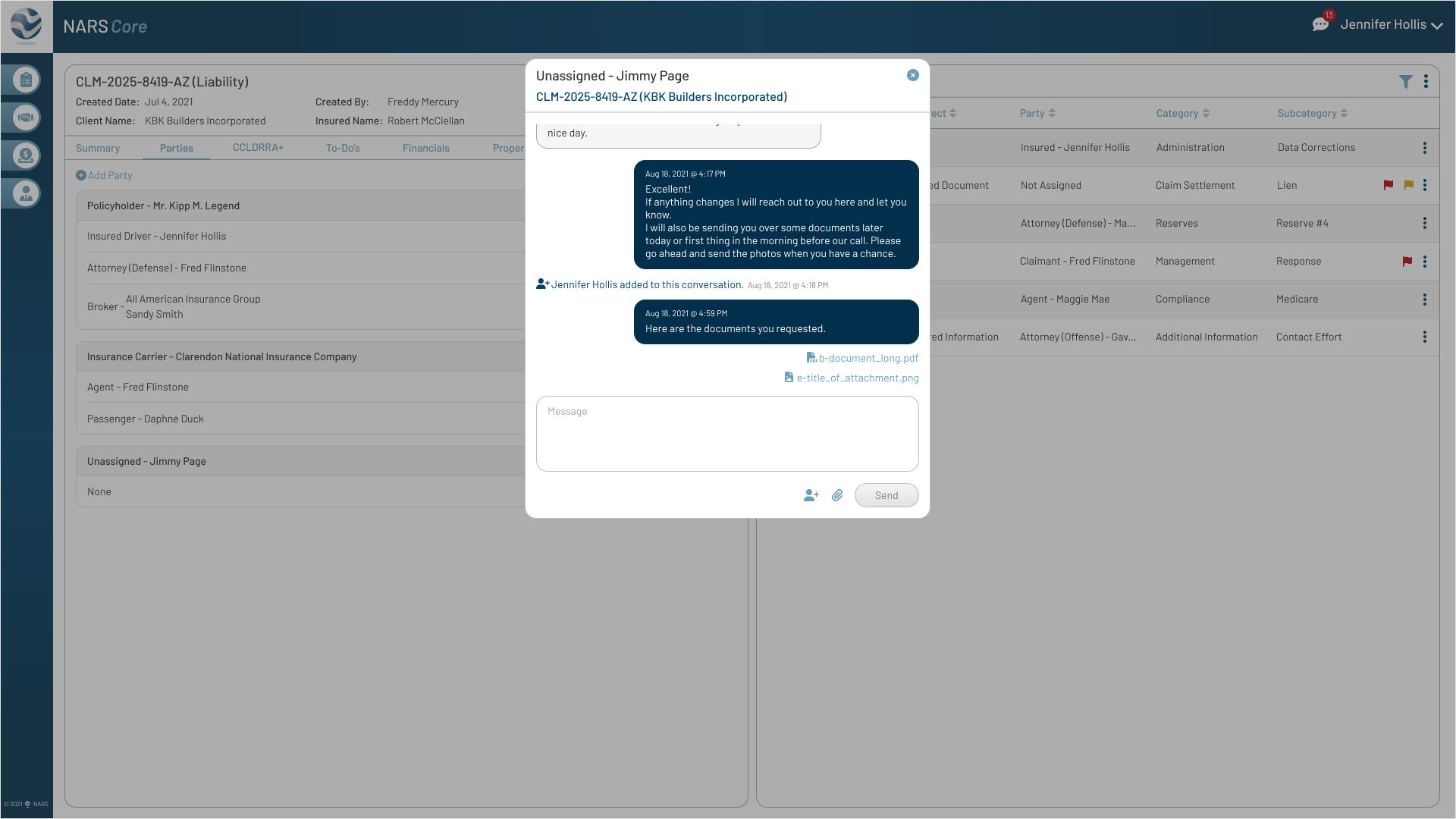
Feedback
The original messaging pattern assumed one-to-one conversations, but complex claims often involved multiple adjusters.
Iteration
Allowed adjusters to add participants to an existing thread so claim communication stayed in one traceable history.
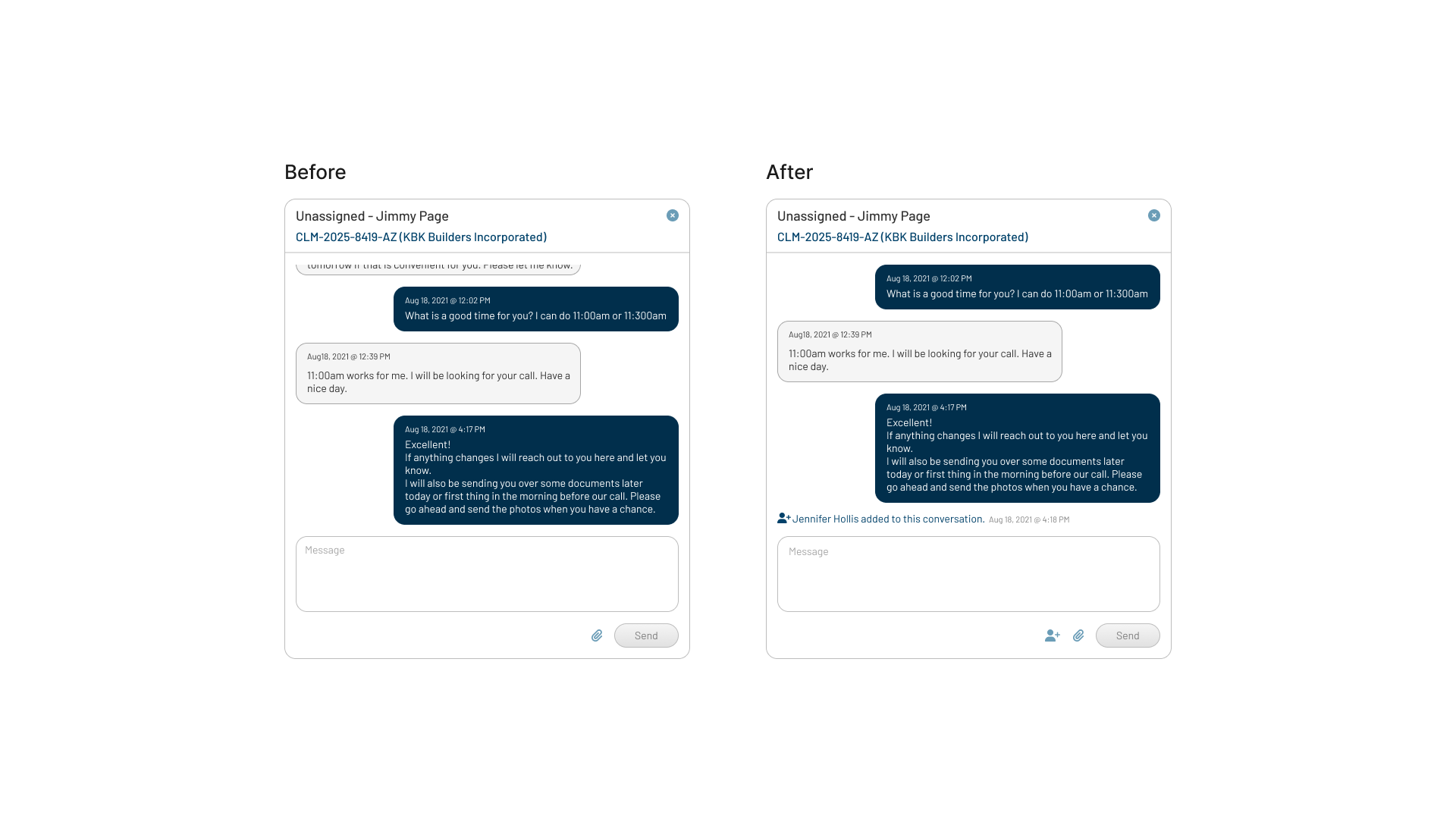
Click to View Image
The final MVP, later piloted as NARS Core, transformed disconnected Claims Cube (C3) workflows into a centralized operational workspace designed around how adjusters actually process claims.
Instead of forcing users through siloed screens, manual tracking, and scattered handoffs, the product brought claim handling, documentation, communication, task management, and parties into a more structured workflow model.
The solution prioritized scannability, task predictability, and operational efficiency. Every major product decision focused on reducing unnecessary navigation, improving task awareness, and helping adjusters maintain context without relying on memory, side notes, or disconnected C3 patterns.
What Changed
Brought claims, tasks, documents, communication, and parties into one shared workspace.
What Changed
Organized dense claim data into predictable layouts that supported high-volume claim work.
What Changed
Added guided actions, documentation support, and visibility cues for required claim work.
What Changed
Built reusable components and implementation-aligned patterns for future platform growth.
This final workspace shows how the MVP translated the approved workflow strategy into a claim-centered experience. Key claim details, task indicators, documentation, parties, and communication patterns were designed to stay connected so adjusters could scan, access, and act from one place.

Annotated NARS Core screen showing how the final MVP brought claim context, documentation, required actions, parties, and communication into a more connected workflow.
The visual system focused less on decoration and more on operational usability.
Because adjusters spent long periods inside high-volume workflows, the interface prioritized accessibility, repeatable patterns, reduced visual noise, and fast scanning over unnecessary visual complexity.
Typography, spacing, color, table structure, and component behavior were designed to support faster information processing, reduce cognitive fatigue, and create predictable workflow patterns across the MVP.
Applied WCAG 2.1 AA contrast, readable states, keyboard considerations, and clear interaction feedback across the system.
Created reusable layouts and components so users could build familiarity across claims, tasks, and documents.
Used color, emphasis, and alerts intentionally so urgent information stood out without overwhelming the workspace.
Designed tables, summaries, and panels for fast scanning, clear comparison, and confident decision-making.
The color palette was designed for heads-down, high-focus claim work while staying aligned with the NARS brand.
Deep blues and structured neutrals supported long reading sessions and dense data review. Semantic colors for alerts, success, and status were used intentionally so urgent items stood out without making the UI feel noisy.
All color decisions were tested against WCAG 2.1 AA contrast standards to support readability, accessibility, and fast recognition of system states.
Primary

Secondary

Grayscale

While NARS traditionally used Optima Pro in print, the product team standardized on Barlow for the Claim Processing Application to better support screen-based, data-heavy workflows.
Barlow’s open counters, generous x-height, and clean geometry created a stronger hierarchy across tables, forms, and multi-column layouts. This helped adjusters scan quickly, maintain context, and work through dense claim information with less visual strain.
Barlow

Because the MVP was expanding across interconnected workflows, consistency became critical early in the process.
I created a scalable Figma design system that aligned closely with Angular implementation patterns, helping engineering move faster while keeping the experience visually and behaviorally consistent.
The system acted as the bridge between design and development. It included reusable components, tokenized styles, spacing standards, typography hierarchy, interaction states, and accessibility-conscious patterns that could scale across future releases.
I also partnered closely with engineering inside VS Code and Angular-based workflows to ensure components, tokens, and interaction patterns translated cleanly from Figma into implementation. This reduced duplicated design effort, improved handoff clarity, and contributed to an 80% increase in development velocity across the MVP.
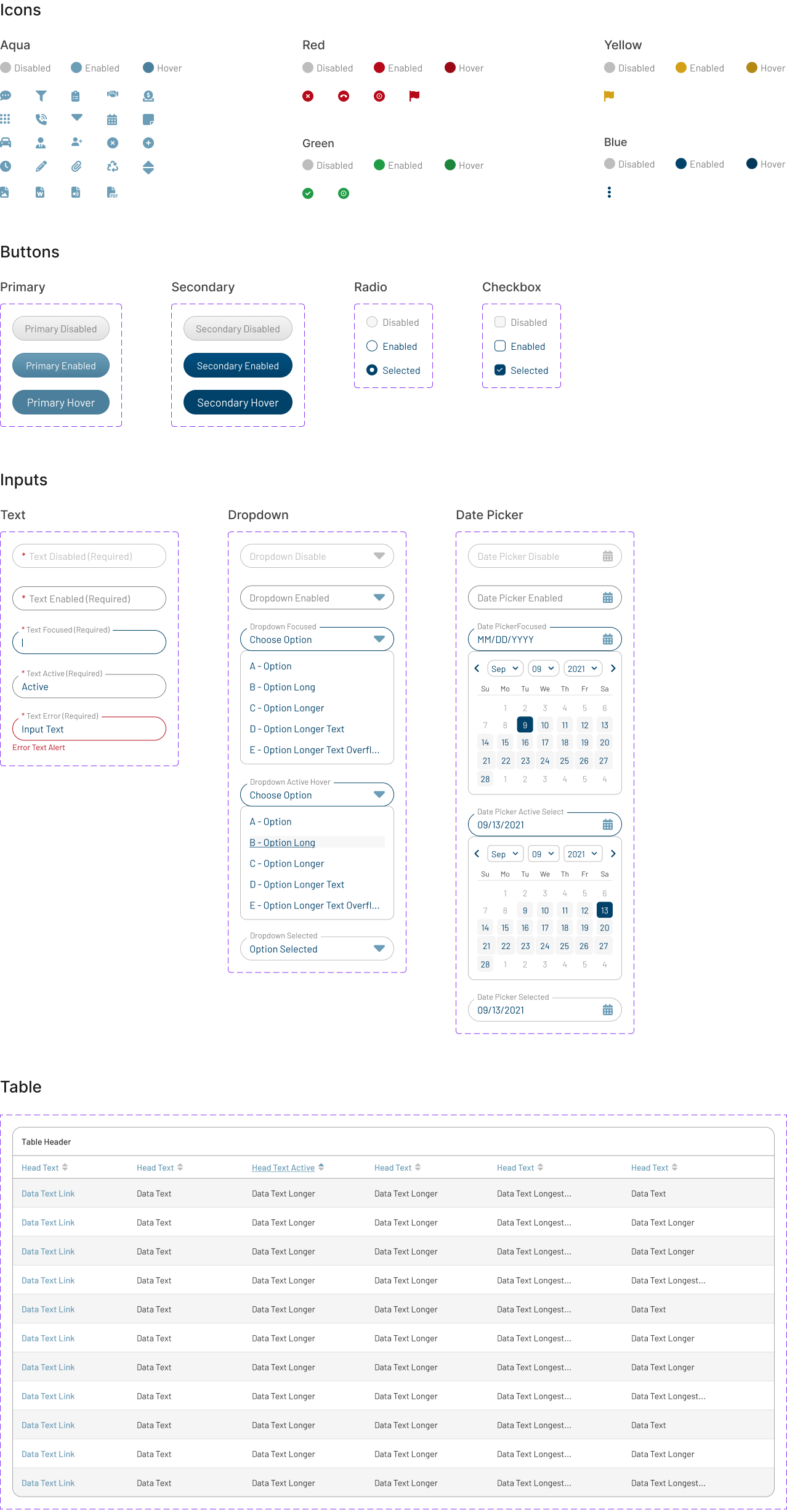
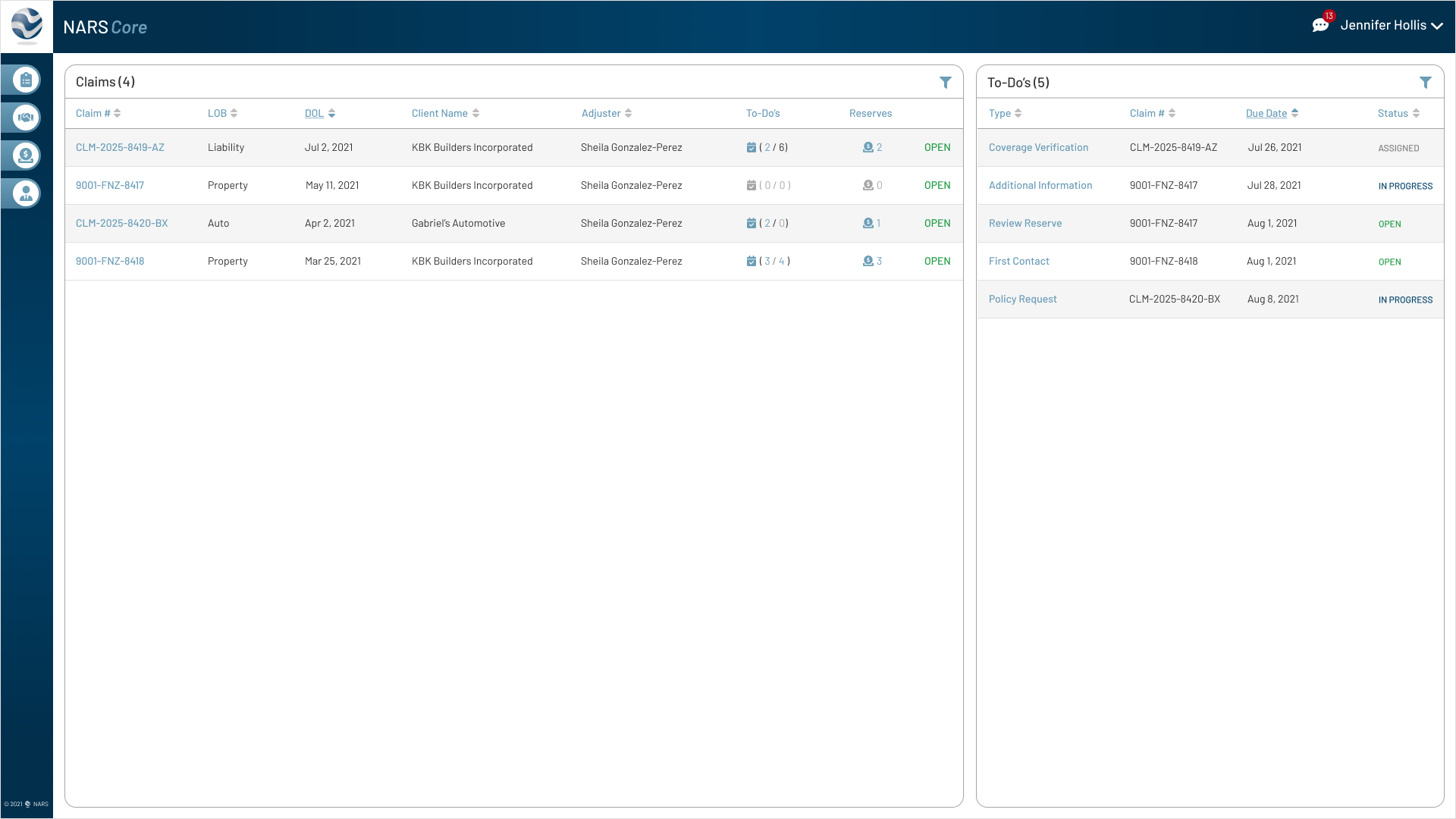
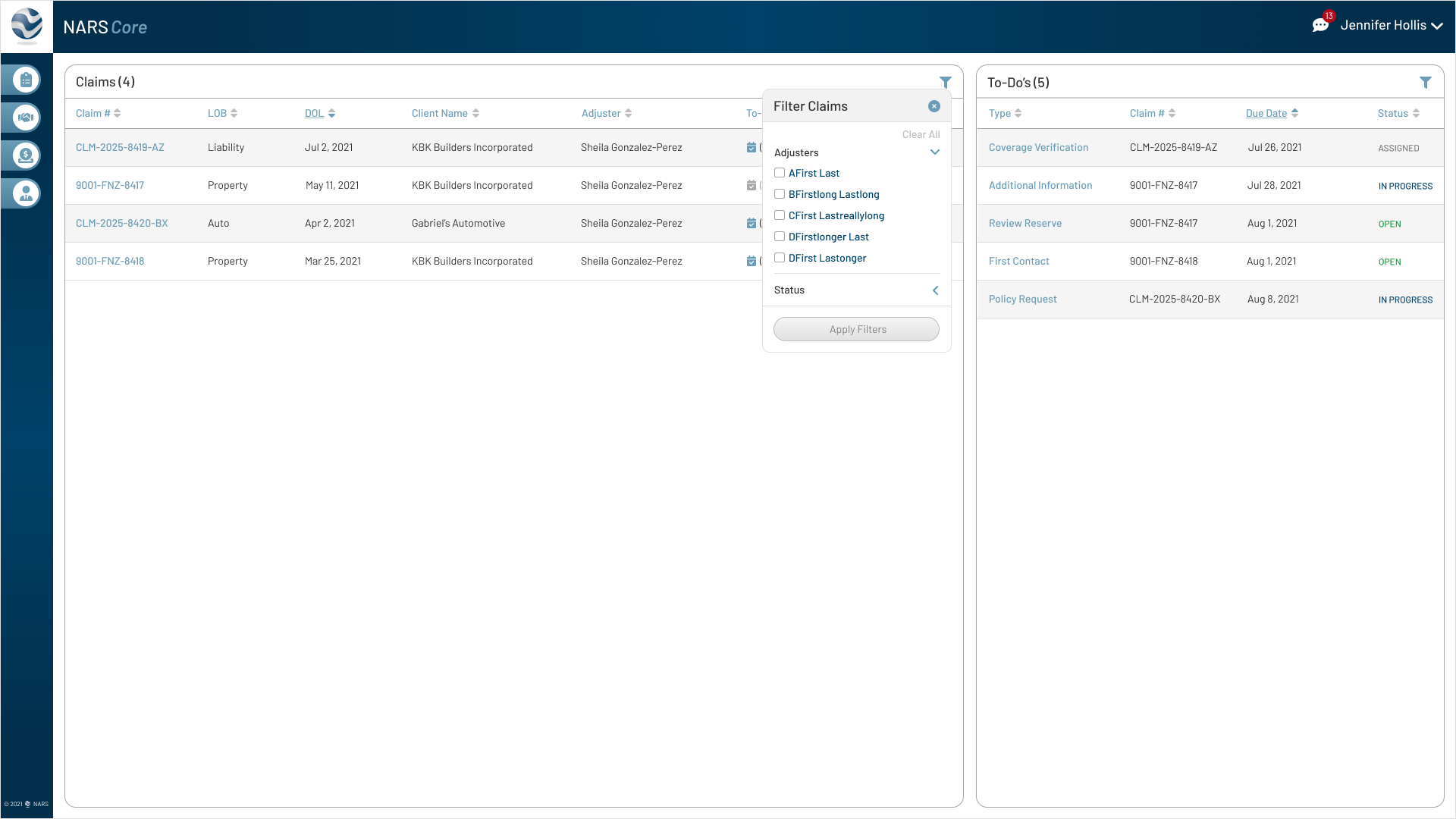
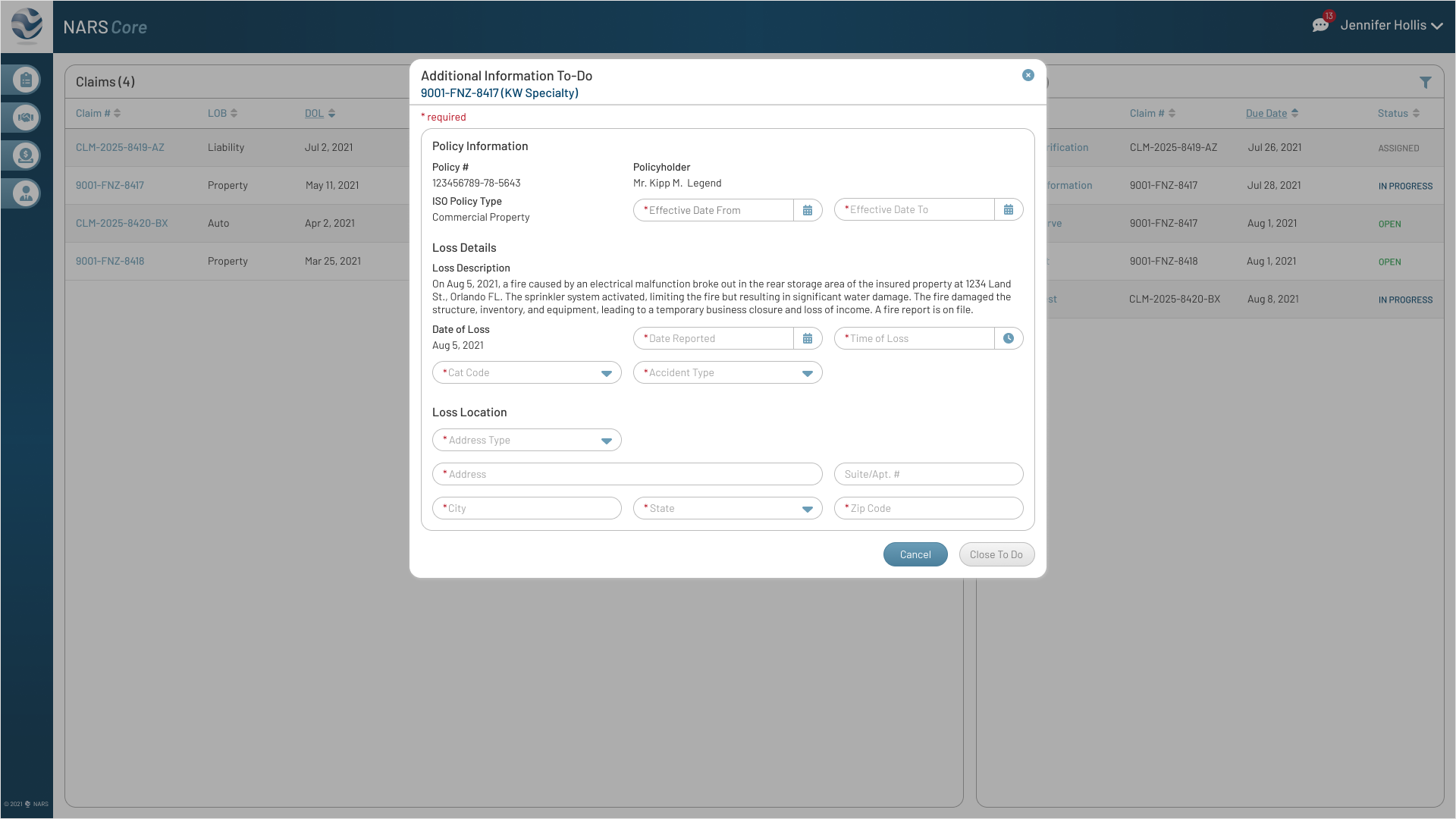
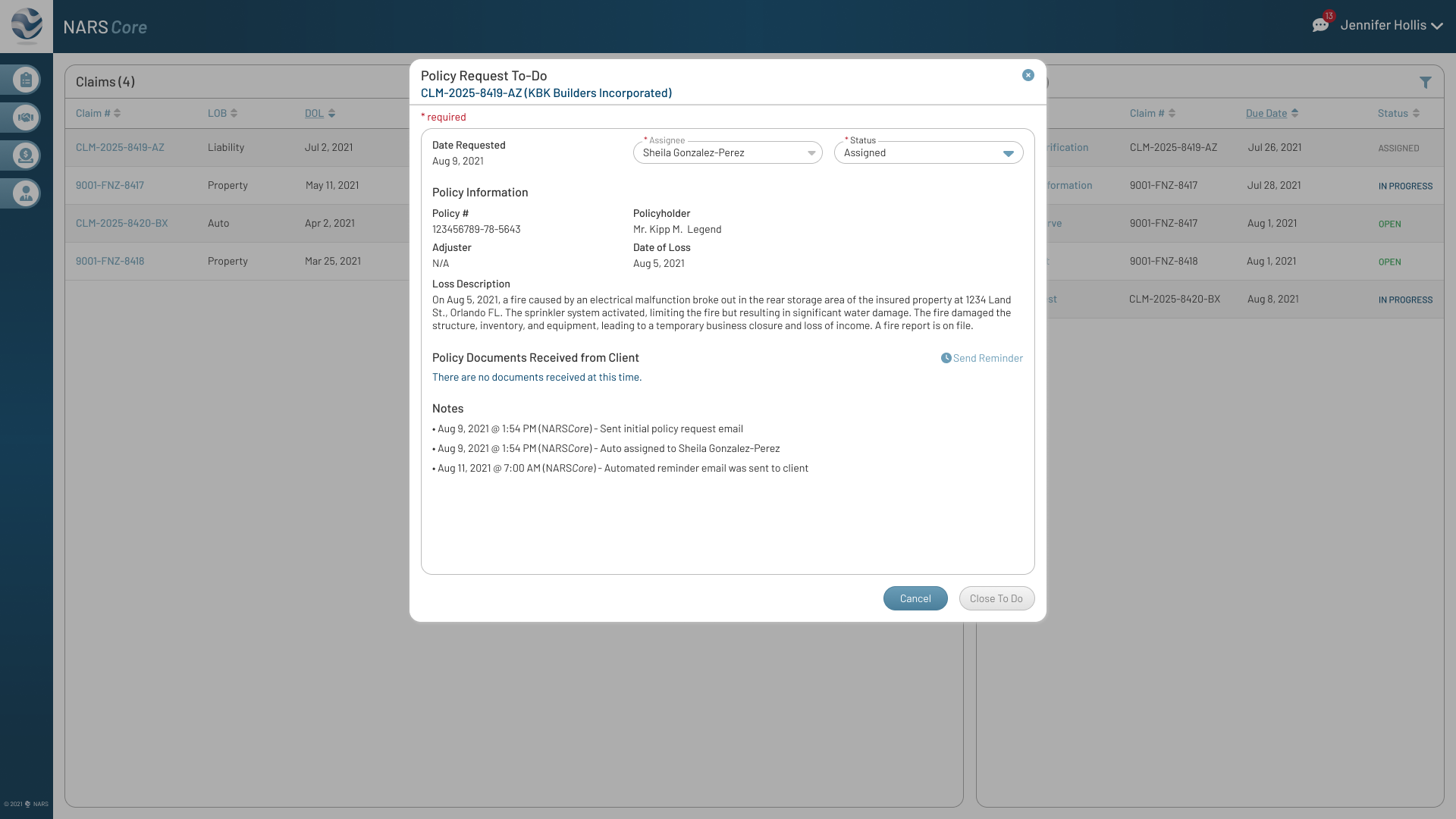
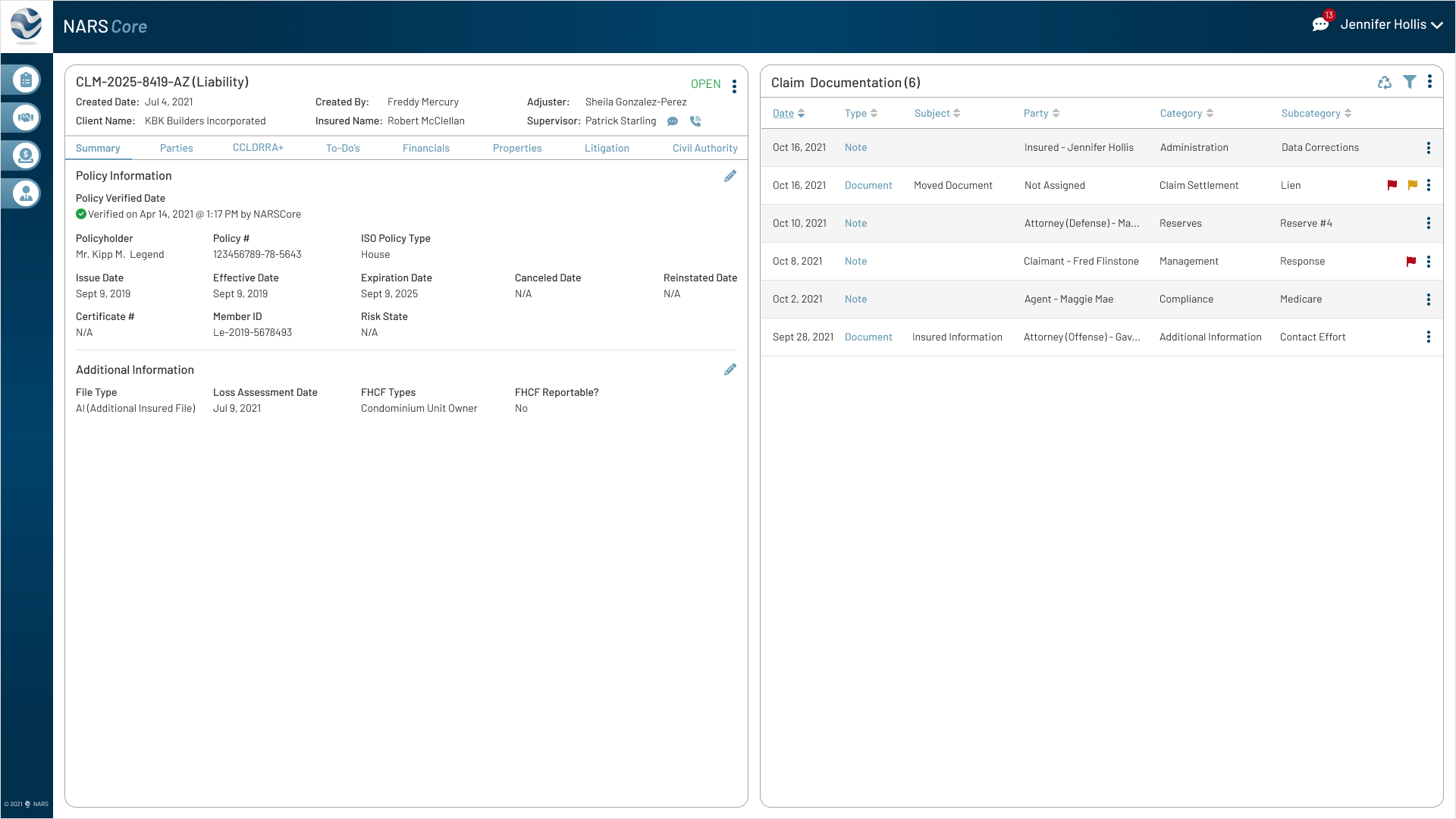
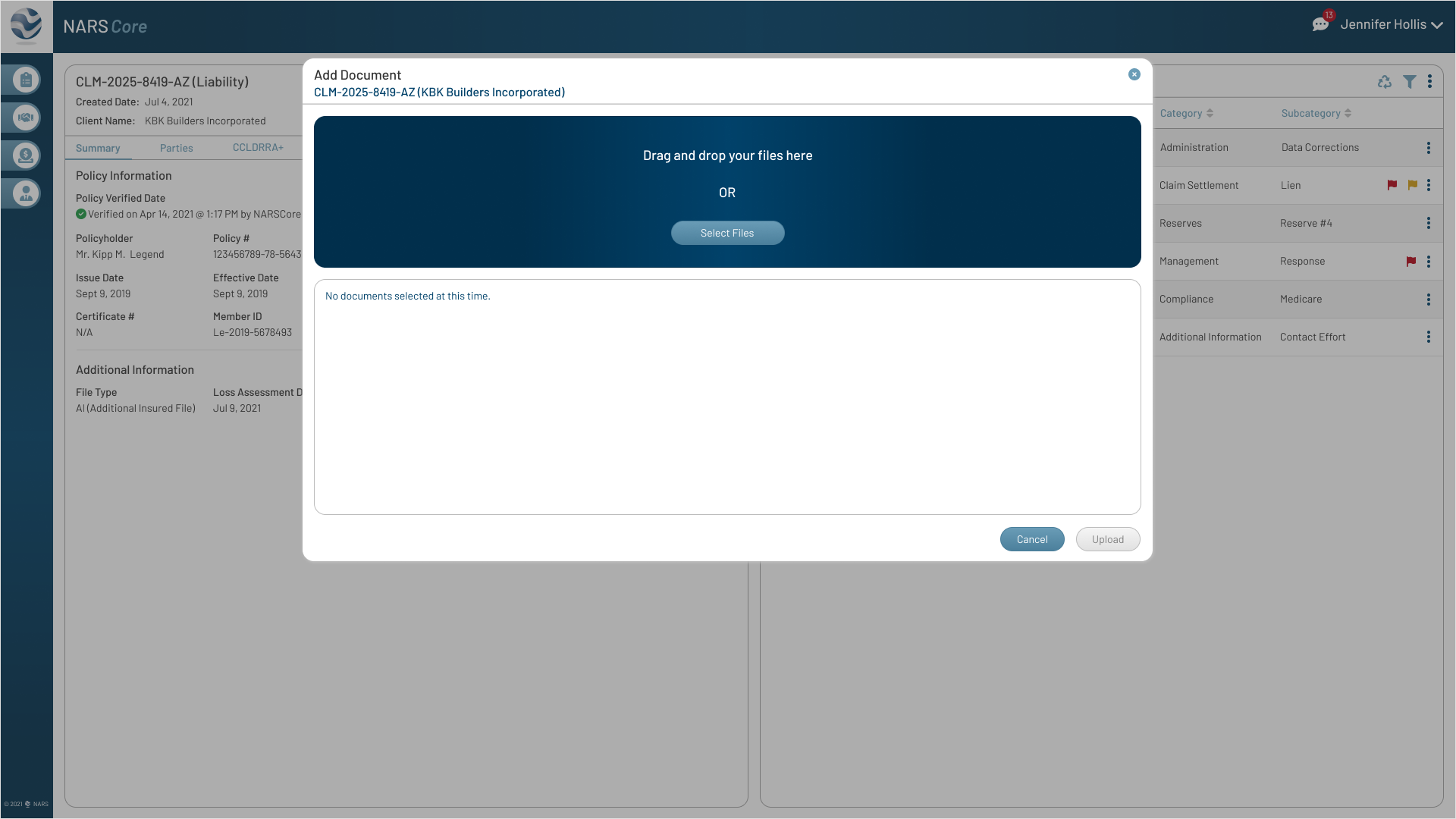
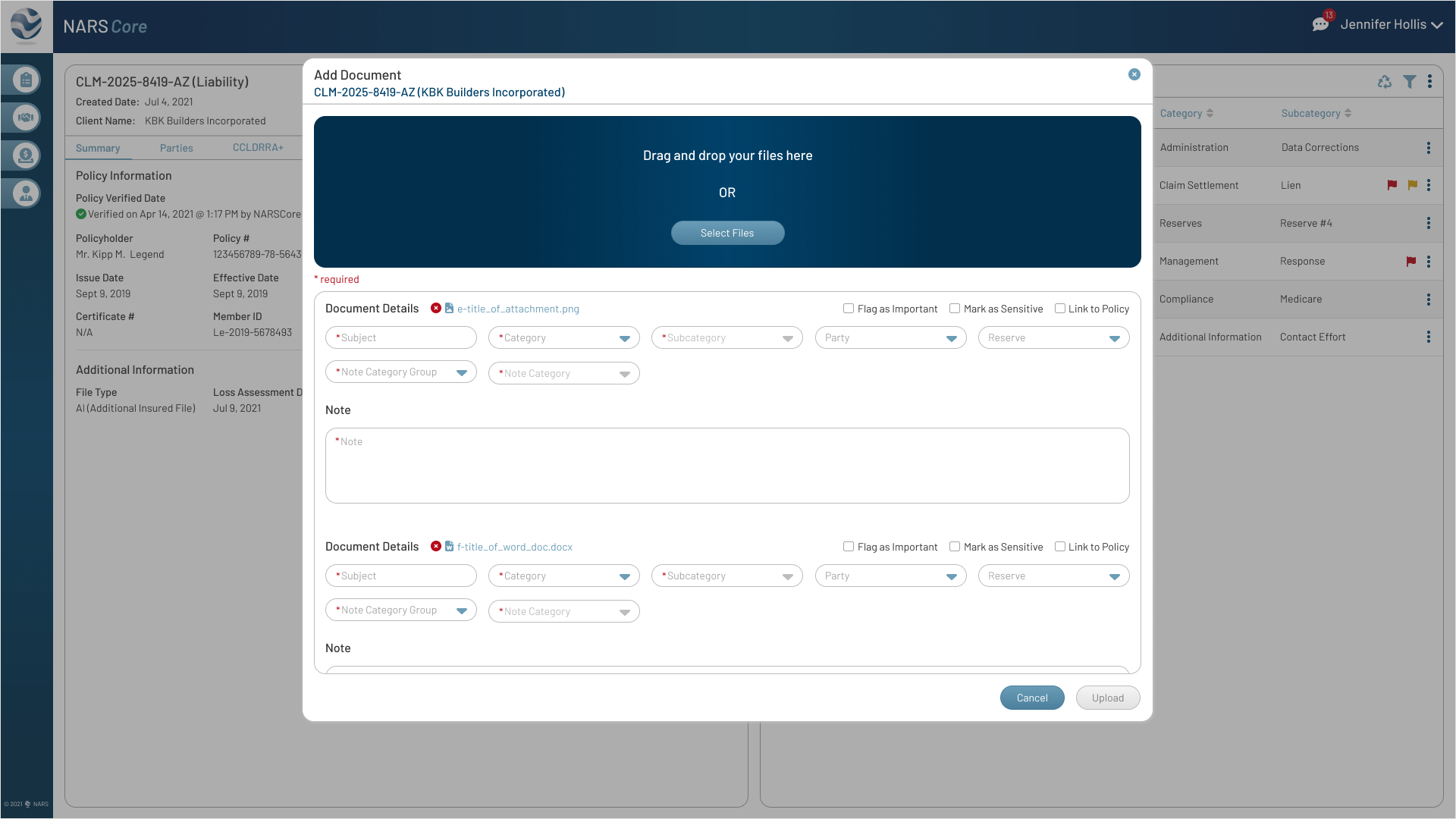
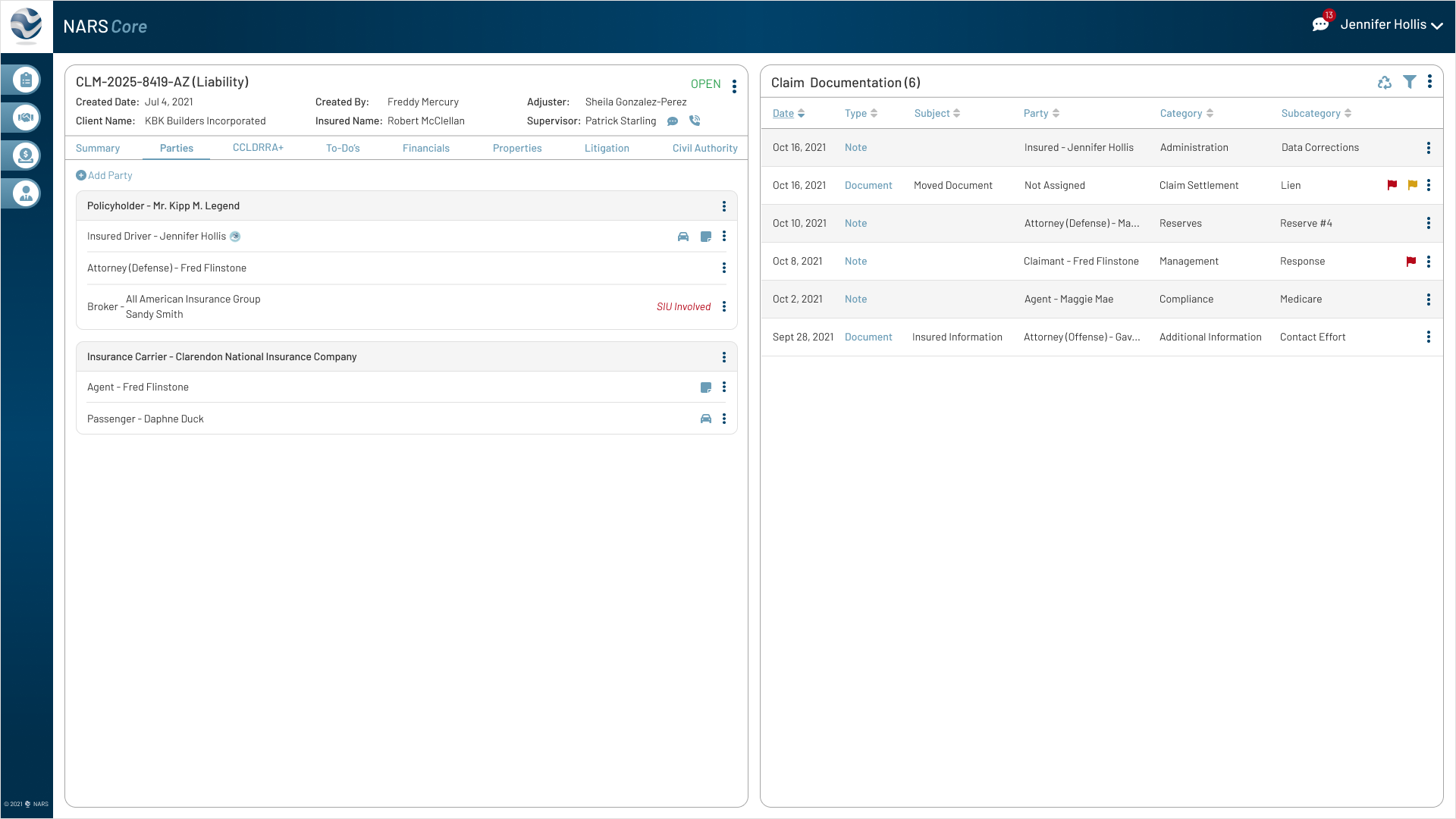
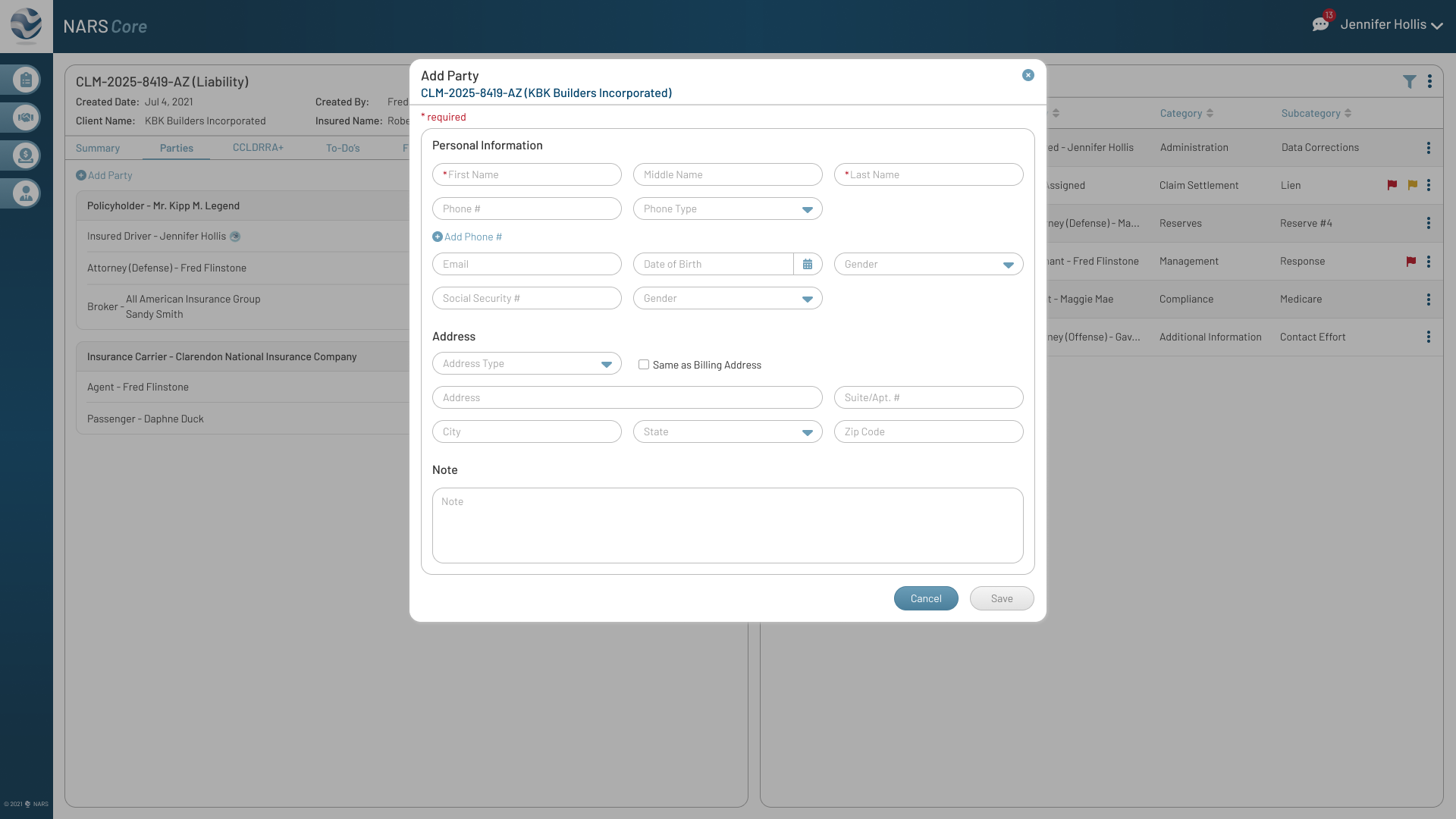
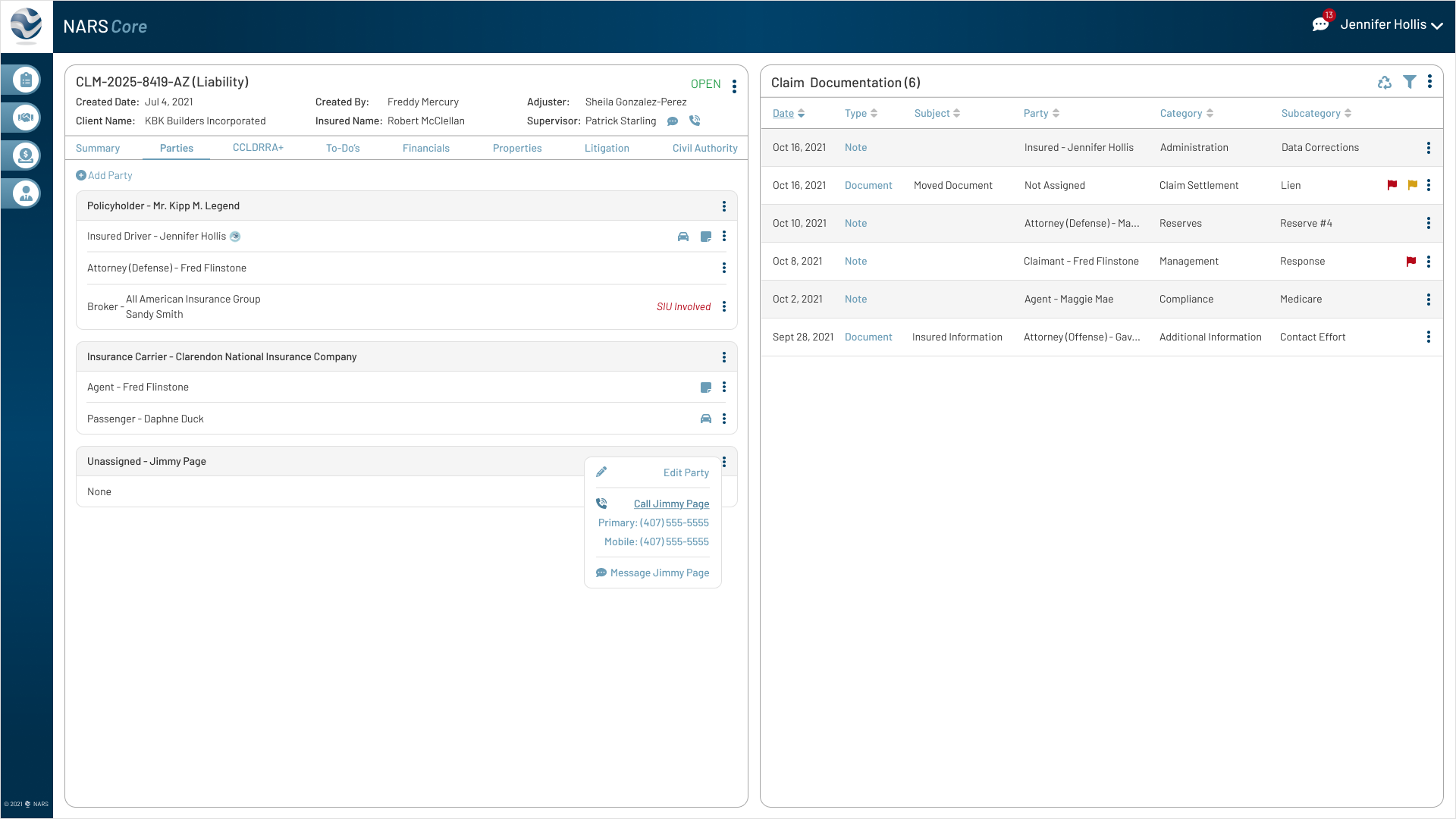
The final designs expanded the MVP across the core workflows adjusters needed most: secure login, claim landing, filtering, to-dos, documents, parties, calling, messaging, and shared communication history.
Together, these screens show how NARS Core translated the product strategy into a scalable, accessible claims workspace.
Browse the final MVP screens across the primary claim workflows.

This project reinforced that successful enterprise products are rarely solved through interface design alone.
The larger challenge was creating operational structure: aligning teams around workflow priorities, reducing ambiguity, balancing technical constraints, and designing a system users could realistically adopt under high-volume, compliance-driven conditions.
Several ideas explored during ideation intentionally did not move forward in the MVP. Dashboard-heavy views offered broader visibility, but they added complexity and implementation overhead. Prioritizing a focused claim-first experience created a clearer workflow foundation, reduced scope risk, and better supported the tasks adjusters handled every day.
This work blended product strategy, systems thinking, and hands-on execution. I helped move the team from scattered C3 workflows to a unified MVP foundation that improved clarity for users and gave the product team a scalable path forward.
Above all, this project reaffirmed that great design is not about adding more interface. It is about giving people the clarity, structure, and confidence to move through complex work without feeling overwhelmed.
Helping adjusters regain control of their workflow — and feel supported instead of overwhelmed — was the moment where the work moved beyond screens and became something more meaningful.
It felt like catching the perfect wave 🌊 — when user insight, product direction, systems thinking, and execution finally moved together.
Looking back, I would bring lightweight adjuster-facing validation into the process earlier. Stakeholder and unit manager reviews helped guide the MVP, but earlier prototype feedback from end users could have surfaced workflow refinements sooner around documentation, messaging, and task sequencing.
The MVP created a clear shift in clarity, efficiency, and workflow predictability. What once required adjusters to move through disconnected C3 patterns now functions as a centralized workspace they can rely on.
Pilot reviewers highlighted clearer workflows, reduced screen switching, and a structure that better reflected how adjusters prefer to work. Full end-user testing was planned for Phase II, but early feedback showed strong confidence in the product direction and excitement around where the platform could go next.
“This MVP is already solving problems we’ve lived with for years. I’m really excited to see it grow — and I can’t wait for our teams to start using it once Phase II rolls out. It’s a huge step in the right direction.”
Laura Bennett – Unit Manager, Auto Claims
While Phase I established the foundation, it also clarified opportunities for future platform growth. Several workflows were intentionally kept lightweight to support adoption, implementation speed, and MVP stability before expanding into more advanced operational capabilities.
Phase II focused on evolving the Claim Processing Application from a successful MVP into a more refined, scalable everyday tool for adjusters.
With the core workflow foundation in place, the next phase centered on improving navigation, strengthening claim context, reclaiming screen space for high-value data, and refining the interface around how adjusters handled more complex claim scenarios.
The goal was not to reinvent the product. It was to build on the MVP by making the experience more intuitive, more efficient, and better prepared for expanded features like Search, Notifications, Reserves, and Payments.
Coming Very Soon: Claim Processing Application – UI Redesign & Experience Refinement (Phase II)
Want a sneak peek?
 View NARS (Phase II) final designs – “UI Redesign & Experience Refinement”
View NARS (Phase II) final designs – “UI Redesign & Experience Refinement”

Thank you for your time & consideration. 🙏🏻
Good design earns trust — by making complex work feel clear, actionable, and calm.